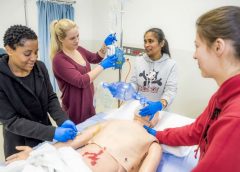
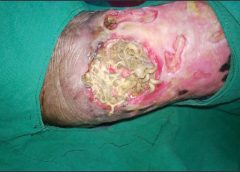
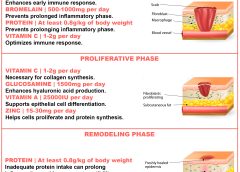
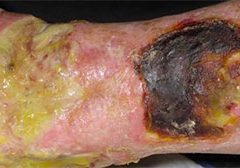
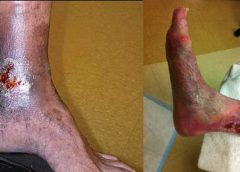
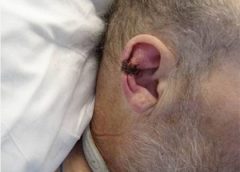
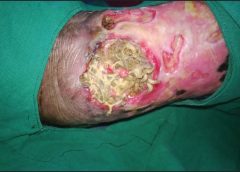
One of the most important steps in achieving positive wound-healing outcomes is to choose the right wound care product. This can be tricky, challenging, and sometimes overwhelming—especially if you’re new to wound care. When I first started in wound care, I had four to five “go-to” products that I knew about. Beyond that, I had to guess what would work. But I learned one thing early: I could call on my sales representatives for help. (more…)
Read MoreSearch Results for: cms
2015 Journal: January – February Vol. 4 No. 1
Healthcare reform and changes provide opportunities for wound care clinicians
By Kathleen D. Schaum, MS
Qualified healthcare professionals (QHPs), such as physicians, podiatrists, physician assistants, nurse practitioners, and clinical nurse specialists, are taught to diagnose the reasons that chronic wounds aren’t healing and to create plans of care for aggressively managing the wound until it heals. Wound care professionals—nurses and therapists—are taught to implement those plans of care. All of these highly skilled wound care professionals know how to manage chronic wounds from identification through healing. (more…)
Read MoreClinician Resources: MRSA, Dosing Calculator, CDC Resources
The Buzz Report: A wound care clinician’s best friend
By Donna Sardina, RN, MHA, WCC, CWCMS, DWC, OMS
In 2014, more than 8,000 new articles related to wound healing were added to the PubMed online database and hundreds of new patents for topical wound formulations were filed. Staying up-to-date with the latest and greatest findings and products can be challenging. We all lead busy lives, and our demanding work schedules and home responsibilities can thwart our best intentions. Although we know it’s our responsibility to stay abreast of changes in our field, we may feel overwhelmed trying to make that happen. (more…)
Read MoreAn easy tool for tracking pressure ulcer data
By David L. Johnson, NHA, RAC-CT
As a senior quality improvement specialist with IPRO, the Quality Improvement Organization for New York State over the past 11 years, I’ve been tasked with helping skilled nursing facilities (SNFs) embrace the process of continuous quality improvement. A necessary component of this effort has been to collect, understand, and analyze timely and accurate data. This article discusses a free tool I developed to help SNFs track their data related to pressure ulcers and focus their quality improvement efforts for the greatest impact. (more…)
Read MoreWhen should we take “No” for an answer?
By: Donna Sardina, RN, MHA, WCC, CWCMS, DWC, OMS
Have you ever had a patient yell “Get out of my room!” or “Don’t touch me! I don’t want to be turned”? How about “No! Don’t put those compression stockings on my legs!” or “No, I’m not going to wear those ugly orthopedic shoes!” or “No way. I can’t stay in bed. I have to go to Bingo!”?
As clinicians, our first instinct usually is paternalistic, as if we’re the patient’s parent who knows what’s best for our child. We think, “Sorry, but you have to do this. It’s for your own good.” And we convey that idea to the patient. (more…)
Read More2014 Journal: November – December Vol. 3 No. 6
2014 Journal: September – October Vol. 3 No. 5
Best of the best, the sequel
By Donna Sardina, RN, MHA, WCC, CWCMS, DWC, OMS
Welcome to our second annual “Best of the Best” issue of Wound Care Advisor, the official journal of the National Alliance of Wound Care and Ostomy (NAWCO). This may be the first time you have held Wound Care Advisor in your hands because normally we come to you via the Internet. Using a digital format for this peer-reviewed journal allows us to bring you practical information that you can access anytime, anywhere and gives you the ability to access videos and other links to valuable resources for you and your patients. (more…)
Read MoreDevice–related pressure ulcers: Avoidable or not?
By: Donna Sardina, RN, MHA, WCC, CWCMS, DWC, OMS
A medical device–related pressure ulcer (MDRPU) is defined as a localized injury to the skin or underlying tissue resulting from sustained pressure caused by a medical device, such as a brace; splint; cast; respiratory mask or tubing; tracheostomy tube, collar, or strap; feeding tube; or a negative-pressure wound therapy device. The golden rule of pressure ulcer treatment is to identify the cause of pressure and remove it. Unfortunately, many of the medical devices are needed to sustain the patient’s life, so they can’t be removed. (more…)
Read More