http://www.npuap.org/world-wide-pressure-ulcer-prevention-day-november-21-2013/
Read MoreMonth: November 2013
Clinician Resources: On the Road Again, Nutrition, Compression
A variety of resources to end the year and take you into 2014.
On the road again
Give your patients with an ostomy this information from the Transportation Security Administration to help them navigate airport screening:
• You can be screened without having to empty or expose your ostomy, but you need to let the officer conducting the screening know about the ostomy before the screening starts.
• You can be screened using imaging technology, a metal detector, or a thorough patdown.
• Your ostomy is subject to additional screening. In most cases, this means you will pat down your ostomy and then your hands will undergo explosive trace detection. (more…)
Making sure patients have the ostomy supplies they need
By Connie Johnson, BSN, RN, WCC, LLE, OMS, DAPWCA
No matter where you work or who your distributors are, ensuring the patient has sufficient ostomy supplies can be a challenge. Whether you’re the nurse, the physician, the patient, or the family, not having supplies for treatments can heighten frustration with an already challenging situation, such as a new ostomy. Here’s how to reduce the chance of experiencing frustrations related to ostomy supplies. (more…)
Read MoreMaking professional connections
By Kathleen D. Pagana, PhD, RN
Are you making connections that benefit your career? Are you comfortable starting a conversation at a networking session? Do you know how to exit a conversation gracefully when it’s time to move on?
These are questions and concerns many clinicians share. Career success takes more than clinical expertise, management savvy, and leadership skills. Networking can be the critical link to success. This article helps you improve your networking skills by focusing on what to do before, during, and after a networking opportunity. (more…)
Read MoreHow do you prove a wound was unavoidable?
By Jeri Lundgren, BSN, RN, PHN, CWS, CWCN
A pressure ulcer that a patient acquires in your facility or a patient’s existing pressure ulcer that worsens puts your organization at risk for regulatory citations as well as litigation. Unless you can prove the pressure ulcer was unavoidable, you could find yourself burdened with citations or fines, or could even end up in court. (more…)
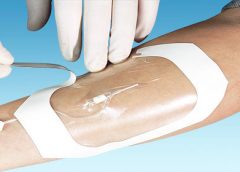
Read MoreWhat you need to know about hydrogel dressings
By Nancy Morgan, RN, BSN, MBA, WOC, WCC, DWC, OMS
Each issue, Apple Bites brings you a tool you can apply in your daily practice.
Description
Hydrated polymer (hydrogel) dressings, originally developed in the 1950s, contain 90% water in a gel base, which helps regulate fluid exchange from the wound surface. Hydrogel dressing are usually clear or translucent and vary in viscosity or thickness. They’re available in three forms: (more…)
Read MoreThe long and short of it: Understanding compression bandaging
By Robyn Bjork, MPT, WCC, CWS, CLT-LANA
Margery Smith, age 82, arrives at your wound clinic for treatment of a shallow, painful ulcer on the lateral aspect of her right lower leg. On examination, you notice weeping and redness of both lower legs, 3+ pitting edema, several blisters, and considerable denudement of the periwound skin. She is wearing tennis shoes and her feet have relatively little edema, but her ankles are bulging over the edges of her shoes; both socks are wet. Stemmer’s sign is negative. The wound on the right leg is draining copious amounts of clear fluid; it’s dressed with an alginate, which is secured with conforming roll gauze. No signs or symptoms of infection are present. (more…)
Read MoreClinical Notes: Pressure-Ulcer Data, Diabetic Foot Ulcers, IFG & HbA1c
Hospital pressure-ulcer comparison data not accurate
Performance scores for rates of hospital-acquired pressure ulcers might not be appropriate for comparing hospitals, according to a study in the Annals of Internal Medicine.
“Hospital report cards for hospital-acquired pressure ulcers: How good are the grades?,” funded by the Agency for Healthcare Research and Quality, analyzed 2 million all-payer administrative records from 448 California hospitals and quarterly hospital surveillance data from 213 hospitals from the Collaborative Alliance for Nursing Outcomes. (more…)
Read MoreProtecting yourself from a job layoff
by Donna Sardina, RN, MHA, WCC, CWCMS, DWC, OMS
With uncertainty over how the Affordable Care Act (ACA) ultimately will affect operations, hospitals and other healthcare facilities are tightening up. In many areas, they’re laying off staff. In May, the healthcare industry lost 9,000 jobs—the worst month for the industry in a decade—and another 4,000 jobs were lost in July.
Medicare, Medicaid, and private insurance companies are reducing reimbursements to care providers, meaning less money is coming in and healthcare facilities have less money to pay out. In my experience, when job cuts are needed, the specialty and subspecialty positions go first. Wound and ostomy care is a subspecialty, so we need to be prepared to protect our jobs—not only for ourselves but for our patients. (more…)
Read MoreSkin problems with chronic venous insufficiency and phlebolymphedema
Dermatologic difficulties: Skin problems in patients with chronic venous insufficiency and phlebolymphedema By Nancy Chatham, RN, MSN, ANP-BC, CWOCN, CWS; Lori Thomas, MS, OTR/L, CLT-LANA; and Michael Molyneaux, MD
Skin problems associated with chronic venous insufficiency (CVI) and phlebolymphedema are common and often difficult to treat. The CVI cycle of skin and soft tissue injury from chronic disease processes can be unrelenting. If not properly identified and treated, these skin problems can impede the prompt treatment of lymphedema and reduce a patient’s quality of life.
This article reviews skin problems that occur in patients with CVI and phlebolymphedema and discusses the importance of using a multidisciplinary team approach to manage these patients. (more…)
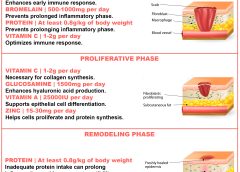
Read MoreHow dietary protein intake promotes wound healing
By Nancy Collins, PhD, RD, LD/N, FAPWCA, and Allison Schnitzer
Nutrition is a critical factor in the wound healing process, with adequate protein intake essential to the successful healing of a wound. Patients with both chronic and acute wounds, such as postsurgical wounds or pressure ulcers, require an increased amount of protein to ensure complete and timely healing of their wounds.
Elderly patients with wounds pose a special challenge because of their decreased lean body mass and the likelihood of chronic illnesses and insufficient dietary protein intake. To promote a full recovery, wound care clinicians must address the increased protein needs of wound patients, especially elderly patients. (more…)
Read More