Month: November 2015
November/December 2015
Time to select a support surface
By Donna Sardina, RN, MHA, WCC, CWCMS, DWC, OMS
Having the proper support surface for beds and wheelchairs is imperative in preventing pressure ulcers. “Pressure” ulcers are named that for a reason—pressure is the primary cause of interruption of blood flow to the tissue. Unfortunately, guidelines for support surface selection tend to make recommendations for the type of surface to use after a pressure ulcer has developed. Another factor that complicates matters is the development of deep-tissue injuries. These injuries start at the bone level, which means that often, tissue damage is extensive before we see visible signs and realize that the support surface we chose might not have been effective enough. (more…)
Read MoreProve the Value Program
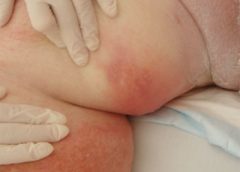
Cutaneous candidiasis
By Nancy Morgan, RN, BSN, MBA, WOC, WCC, DWC, OMS
Each issue, Apple Bites brings you a tool you can apply in your daily practice. Here’s an overview of cutaneous candidiasis.
Cutaneous candidiasis is an infection of the skin caused by the yeast Candida albicans or other Candida species. Here’s a snapshot of this condition. (more…)
Read MoreClinical Notes: Modified Braden Risk Score, dialysis patients, plantar
Modified Braden risk score proposed
A study in Ostomy Wound Management states the risk classification of patients using Braden Scale scores should comprise three (rather than five) levels: high risk, with a total score ≤11; moderate risk, with a total score of 12 to 16; and mild risk, with a total score ≥17.
The retrospective analysis of consecutively admitted patients at risk for pressure ulcer to an acute-care facility included 2,625 patients, with an age range from 1 month to 98 years; 3.1% developed a pressure ulcer. (more…)
Read MoreSeeing healthcare from a new perspective
By: Donna Sardina, RN, MHA, WCC, CWCMS, DWC, OMS
As healthcare clinicians, our world is full of tasks to be completed. Some are new, but many are tasks we repeat every day and thus have become routine—things we could almost do in our sleep.
But what’s routine for us may not be routine for our patients. For some patients, these routine tasks of ours may be their first encounter with a healthcare situation. (more…)
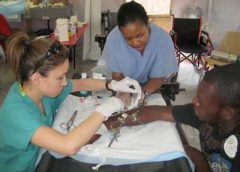
Read MoreProviding skin care for bariatric patients
By Gail R. Hebert, MS, RN CWCN, DWC, WCC, OMS
How would you react if you heard a 600-lb patient was being admitted to your unit? Some healthcare professionals would feel anxious—perhaps because they’ve heard bariatric patients are challenging to care for, or they feel unprepared to provide their care. (more…)
Read MoreRole of the ostomy specialist clinician in ileal pouch anal anastomosis surgery
By Leanne Richbourg, MSN, RN, APRN-BC, CWON-AP, CCCN, GCNS-BC
Restorative proctocolectomy with ileal pouch anal anastomosis (IPAA) is the gold standard for surgical treatment of ulcerative colitis (UC) or familial adenomatous polyposis (FAP). It’s also done to treat colon and rectal cancers, such as those caused by Lynch syndrome (LS). IPAA allows the patient to maintain fecal continence and evacuate stool from the anus after colon and rectum removal. A temporary ileostomy may be part of the overall process, but there’s no need for a permanent stoma. (See Understanding ulcerative colitis, FAP, and Lynch syndrome.) (more…)
Read MoreStaying out of sticky situations: How to choose the right tape for your patient
By Ann-Marie Taroc, MSN, RN, CPN
Are you using the wrong kind of medical tape on your patients? Although we strive to provide the safest care possible, some nurses may not realize that medical tape used to secure tubes and dressings can cause harm. The harm may stem from using the wrong product or using a product incorrectly, which can cause adhesive failure or skin injury. (more…)
Read MoreClinician Resources: falls, npuap, patient safety, civility
End your year by checking out these resources for your practice.
Sentinel event alert for falls
As part of its sentinel event alert “Preventing falls and fall-related injuries in health care facilities,” The Joint Commission has assembled information and multiple resources, including:
- analysis of contributing factors for falls
- evidence-based suggestions for improvement
- Joint Commission requirements relevant to falls
- links to toolkits and protocols
- an infographic on preventing falls.
Is your therapy department on board with your wound care team?
By Cheryl Robillard, PT, WCC, CLT, DWC
Patients in your clinical practice who develop wounds should prompt a call for “all hands on deck” to manage the situation, but some personnel may be missing the boat. Physical therapists (PTs), occupational therapists (OTs), and speech-language pathologists (SLPs) should be on board your wound care ship so patients can receive care they need. But unfortunately, sometimes they aren’t. (more…)
Read More