Support surfaces are consistently recommended for the prevention and treatment of pressure ulcers. So patients can derive optimal benefits from support surfaces, clinicians must understand how to use them effectively. This article answers several questions about these useful tools. (more…)
Read MoreSearch Results for: measur
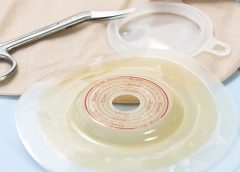
Clinical Notes: ostomy, pressure ulcer, burn treatment
Self-management ostomy program improves HRQOL
A five-session ostomy self-care program with a curriculum based on the Chronic Care Model can improve health-related quality of life (HRQOL), according to a study in Psycho-Oncology.
“A chronic care ostomy self-management program for cancer survivors” describes results from a longitudinal pilot study of 38 people. Participants reported sustained improvements in patient activation, self-efficacy, total HRQOL, and physical and social well-being. Most patients had a history of rectal cancer (60.5%) or bladder cancer (28.9%). (more…)
Read MoreBuzz Report: Latest trends, part 2
Keeping clinicians up-to-date on clinical knowledge is one of the main goals of the Wild on Wounds (WOW) conference held each September in Las Vegas. Every year, I present the opening session, called “The Buzz Report,” which focuses on the latest-breaking wound care news—what’s new, what’s now, and what’s coming up. I discuss new products, practice guidelines, resources, and tools from the last 12 months in skin, wound, and ostomy management.
In the January issue, I discussed some of the updates from my 2015 Buzz Report. Now I’d like to share a few more, along with some of my favorite resources. (more…)
Read MoreEmpowering patients to play an active role in pressure ulcer prevention
Developing a pressure ulcer can cause the patient pain, lead to social isolation, result in reduced mobility, and can even be fatal. According to the Agency for Healthcare Research and Quality, estimated costs for each pressure ulcer range from $37,800 to $70,000, and the total annual cost of pressure ulcers in the United States is an estimated $11 billion.
Nurses understand their role in preventing pressure ulcers, but what role do patients play in the prevention plan? Nurses need to empower the patient to be an active member in health promotion activities and participate in prevention measures. In this article, I highlight the importance of incorporating pressure ulcer prevention into patient education for high-risk patients as a way to empower patients. Empowered patients can help improve outcomes and reduce overall costs of this hospital-acquired complication. (more…)
Read MoreBuzz Report: Latest trends, Part 1
We all lead busy lives, with demanding work schedules and home responsibilities that can thwart our best intentions. Although we know it’s our responsibility to stay abreast of changes in our field, we may feel overwhelmed when we try to make that happen.
Keeping clinicians up-to-date on clinical knowledge is one of the main goals of the Wild On Wounds (WOW) conference, held each September in Las Vegas. Each year, I present the opening session of this conference, called “The Buzz Report,” which focuses on the latest-breaking wound care news—what’s new, what’s now, what’s coming up. I discuss innovative new products, practice guidelines, resources, and tools from the last 12 months in skin, wound, and ostomy management. This article highlights the hottest topics from my 2015 Buzz Report. (more…)
Read MoreClincal Notes: Analysis, Osteomyelitis, sickle cell, maggot
Value of systematic reviews and meta-analyses in wound care
“Systematic reviews and meta-analyses—literature-based recommendations for evaluating strengths, weaknesses, and clinical value,” in Ostomy Wound Management, discusses evidence-based practice and how systematic reviews (SRs) and meta-analyses (MAs) can help improve management of wound care patients.
The authors of the article explain evidence-based practice and provide useful definitions for key terms. They then provide a list of eight questions to use when evaluating SRs and practical tips such as how to search for SR and MA studies. The article finishes with a list of eight interventions supported by the most evidence: hydrocolloidal dressings, honey, biosynthetic dressings, iodine complexes, silver compounds, hydrogels, foam dressings, and negative pressure wound therapy. (more…)
Read MoreClinician Resources: Ulcer Prevention, CAUTI, Negative Bacteria
Start the New Year off right by checking out these resources.
Pressure ulcer prevention education
Access the following education resources from Wounds International:
The webinar “Real-world solutions for pressure ulcer prevention: Optimising the role of support surfaces” includes:
• an overview of the issue of pressure ulcers
• what to consider when choosing a support surface
• how to operationalize support surfaces in the clinical setting. (more…)
Read MoreRole of the ostomy specialist clinician in ileal pouch anal anastomosis surgery
By Leanne Richbourg, MSN, RN, APRN-BC, CWON-AP, CCCN, GCNS-BC
Restorative proctocolectomy with ileal pouch anal anastomosis (IPAA) is the gold standard for surgical treatment of ulcerative colitis (UC) or familial adenomatous polyposis (FAP). It’s also done to treat colon and rectal cancers, such as those caused by Lynch syndrome (LS). IPAA allows the patient to maintain fecal continence and evacuate stool from the anus after colon and rectum removal. A temporary ileostomy may be part of the overall process, but there’s no need for a permanent stoma. (See Understanding ulcerative colitis, FAP, and Lynch syndrome.) (more…)
Read More2015 Journal: Best of the Best Vol. 4 No. 5
A collaborative approach to wound care and lymphedema therapy: Part 2
By Erin Fazzari, MPT, CLT, CWS, DWC
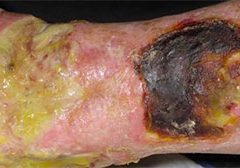
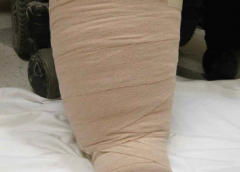
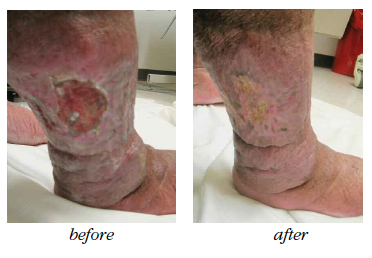
Have you seen legs like these in your practice?
These legs show lymphedema and chronic wounds before treatment (left image) and after treatment (right image) with complex decongestive therapy (CDT)—the gold standard of lymphedema care. The patient benefited from multidisciplinary collaboration between wound care and lymphedema therapists. (more…)
Read MorePreventing pressure ulcers in pediatric patients
By Roxana Reyna, BSN, RNC-NIC, WCC, CWOCN
As wound care clinicians, we are trained—and expected—to help heal wounds in patients of any age and to achieve positive outcomes. Basic wound-healing principles apply to all patients, whatever their age or size. The specific anatomy and physiology of vulnerable pediatric patients, however, requires detailed wound care. Unfortunately, little evidence-based research exists to support and direct the care of pediatric patients with pressure ulcers. This article describes efforts to reduce pressure ulcers in pediatric patients at Driscoll Children’s Hospital (DCH) in Corpus Christi, Texas. (more…)
Read MoreCase study: Early detection and treatment resolves a deep tissue injury
By Todd Zortman, RN, WCC, and James Malec, PhD
Pressure ulcers are a chronic healthcare burden for both patients and providers. Over 2.5 million patients in the United States are affected annually by pressure ulcers, with nearly 60,000 of those cases directly resulting in death. From a provider’s perspective, the cost of individual care ranges anywhere from $500 to $70,000 per pressure ulcer, which translates to annual costs in the U.S. approaching $11 billion. (more…)
Read More