Search Results for: Dr
White House declares war on drug-resistant superbugs
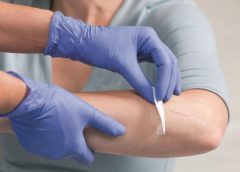
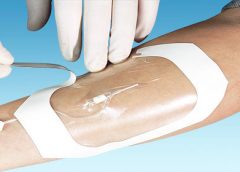
What you need to know about transparent film dressings
By Nancy Morgan, RN, BSN, MBA, WOC, WCC, DWC, OMS
Each issue, Apple Bites brings you a tool you can apply in your daily practice.
Transparent film dressings are thin sheets of transparent polyurethane (polymer) coated with an adhesive. These dressings are available in a variety of sizes and shapes. (more…)
Read MoreWhat you need to know about hydrogel dressings
By Nancy Morgan, RN, BSN, MBA, WOC, WCC, DWC, OMS
Each issue, Apple Bites brings you a tool you can apply in your daily practice.
Description
Hydrated polymer (hydrogel) dressings, originally developed in the 1950s, contain 90% water in a gel base, which helps regulate fluid exchange from the wound surface. Hydrogel dressing are usually clear or translucent and vary in viscosity or thickness. They’re available in three forms: (more…)
Read MoreWhat you need to know about collagen wound dressings
By Nancy Morgan, RN, BSN, MBA, WOC, WCC, DWC, OMS
Description
Collagen, the protein that gives the skin its tensile strength, plays a key role
in each phase of wound healing. It attracts cells, such as fibroblasts and keratinocytes, to the wound, which encourages debridement, angiogenesis, and reepithelialization. In addition, collagen provides a natural scaffold or substrate for new tissue growth. (more…)
Imposter syndrome: when you feel like you’re faking it
By Rose O. Sherman, EdD, RN, NEA-BC, FAAN
Colleen Jackson recently was promoted to a manager position on her unit. At first, she was thrilled with the opportunity to advance her leadership skills, but now she’s having second thoughts. She doesn’t feel confident in her new role and worries how her team views her. She confesses to her manager, “I keep thinking someone will figure out how much I really don’t know and question whether I should’ve been given the position. Sometimes I feel like an imposter. When I mention this to my friends, they tell me to ‘fake it until you make it.’ But I’m not so sure about that!”
Colleen isn’t alone in feeling like an imposter. In imposter syndrome, a person doesn’t feel good enough, is unsure of what she’s doing, and feels she can’t live up to others’ expectations. She may be afraid she’ll be found out as an imposter at any moment. The syndrome is most common among women leaders who feel they don’t deserve the success they’ve achieved despite external evidence of their competence. It’s more likely in perfectionists who constantly compare themselves to others.
Certain situations, such as taking on a new role, can lead to imposter syndrome. For instance, Colleen may think that because she was seen as qualified for her new role, others expect her to immediately have expert knowledge. If, like Colleen, you feel you don’t deserve the career success you’ve had, you may experience deep feelings of inauthenticity and fear you’ll be found out as a fake. (See Inside the imposter syndrome.)
In small doses, feelings of inadequacy may not be a bad thing, because they remind us to work on building our competency. But people with imposter syndrome feel a level of self-doubt that can lead to overwork and a paralyzing fear of failure. The fear of being unmasked causes incredible stress. Colleen and others like her may have unrealistic expectations of themselves in a new role—expectations that can compromise their success.
Overcoming imposter syndrome
For people with imposter syndrome, the response to their success may rest too heavily on others’ approval, recognition, and opinions. A wise mentor once told me we can easily overestimate how much time others spend thinking about us and our behaviors. Most people, she observed, are self-absorbed. This is important to consider, because the idea that Colleen is an imposter probably has never crossed her team members’ minds.
Imposter syndrome can create performance anxiety and lead to perfectionism, burnout, and depression. So learning how to manage these feelings is important. Cathy Robinson-Walker, MBA, MCC, who coaches nurse leaders, provides advice to help cope with imposter syndrome. Her recommendations include the six actions steps below.
Discuss your feelings with a trusted mentor.
Sharing your insecurities with someone you trust and respect can help you separate what’s real from your perceptions of insecurity. A trusted mentor might inform Colleen she’s making good progress as a beginning leader and that no one expects her to be an expert at this point. The mentor can provide guidance about specific areas where Colleen might need additional growth and how to best go about this.
Pay attention to your own self-talk and consider whether your thoughts are empowering or disabling.
Do you often say to yourself, “I achieved this only because I work harder than anyone else, not because I’m more competent”? Valerie Young, author of The Secret Thoughts of Successful Women: Why Capable People Suffer from the Impostor Syndrome and How to Thrive in Spite of It, makes a strong case that your internal script is a well-rehearsed pattern that serves as a key to feelings of being an imposter. She cautions that individuals with imposter syndrome may sabotage themselves as a way of holding back, due to feelings of being a fraud.
Instead, choose a different script and talk yourself down during times of self-doubt. Instead of thinking, “I’m the wrong person for this job,” retrain yourself to say, “I have a lot to offer in this position.”
Make of list your strengths.
Take the time to make a written list your strengths and what you contribute. Ask others for input, and refer to the list in times of self-doubt. If you’re in a new role, remember that you were chosen for a reason. In Colleen’s case, her supervisor saw her leadership potential. Also realize that most people overestimate their abilities; people with imposter syndrome underestimate theirs.
Accept that perfection is unrealistic and costly.
Trying to be perfect and feeling you need to “know it all” is unrealistic and can be costly on a personal level. Perfectionists typically believe anything short of a flawless performance all the time is unacceptable. But none of us can live a mistake-free life; we all make errors. Those with imposter syndrome hold themselves to impossibly high standards and feel shame, insecurity, and low self-esteem when they don’t meet their own expectations. But progress, not perfection, is what really matters.
Know you’ll need to develop your competencies at certain times in your career.
Throughout your career, you’ll go through periods when you’re on a steep learning curve and will need to further develop your competencies. You may feel like a novice and have to work hard to build new competencies.
Be honest about what you know and don’t know, and seek advice from experts on your unit or in your organization. The simple act of saying, “This is new for me, and I’m working hard to learn this role” can be empowering. Colleen, for instance, might be surprised at others’ reactions to hearing this from her. They might perceive her as a more authentic leader.
Be willing to be uncomfortable and move through your fear.
In Fear of Flying, author Erica Jong urges readers engaging in new experiences to feel the fear and do it anyway. Fear is a useful emotion, as long as it doesn’t escalate to the level of paralyzing behaviors. Practice and preparation can help ease new leaders’ fears. The fear of new challenges will never truly go away, but it can be managed.
Building competence leads to competency
People with imposter syndrome generally are intelligent, thoughtful, and capable but lack self-confidence. Over time, clinicians like Colleen will grow out of feeling like an imposter as they build their competency and become more comfortable in their roles. Eleanor Roosevelt said, “I believe that anyone can conquer fear by doing the things he fears to do, provided he keeps doing them until he gets a record of successful experience behind him.” If you feel like an imposter, this is good advice to ponder.
Selected references
Clance PR, Imes S. The imposter phenomenon in high achieving women: dynamics and therapeutic intervention. Psycho Theor, Res and Prac.1978;15(3):241-7.
Jong E. Fear of Flying. Austin, TX: Holt, Reinhart & Winston; 1973.
Robinson-Walker C. The imposter syndrome. Nurs Leader. 2011;9(4):12-13.
Sherman R.O. Imposter syndrome in nursing leadership. Emerging RN Leader: A Leadership Development Blog. May 7, 2012. www.emergingrnleader.com/
imposter-syndrome-in-nursing-leadership/. Accessed February 26, 2013.
Young V. How to feel as bright and capable as everyone seems to think you are: a handbook for women (and men) who doubt their competence…but shouldn’t. ImposterSyndrome.com. 2004. http://
impostorsyndrome.com/_content/How%20to%20Feel%20As%20Bright%20and%20Capable%20As%20Every
one%20Seems%20to%20Think%20You%20Are%20
Workbook.pdf Accessed February 26, 2013.
Young V. The Secret Thoughts of Successful Women: Why Capable People Suffer from the Impostor Syndrome and How to Thrive in Spite of It. New York: Crown Business; 2011.
Rose O. Sherman is an associate professor of nursing and director of the Nursing Leadership Institute at the Christine E. Lynn College of Nursing at Florida Atlantic University in Boca Raton. You can read her blog at www.emergingrnleader.com.
Read MoreWhat you need to know about hydrocolloid dressings
By Nancy Morgan, RN, BSN, MBA, WOC, WCC, DWC, OMS
Each month, Apple Bites brings you a tool you can apply in your daily practice.
Description
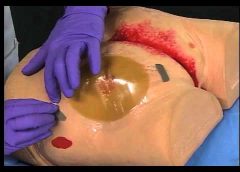
A hydrocolloid dressing is a wafer type of dressing that contains gel-forming agents in an adhesive compound laminated onto a flexible, water-resistant outer layer. Some formulations contain an alginate to increase absorption capabilities. The wafers are self-adhering and available with or without an adhesive border and in various thicknesses and precut shapes for such body areas as the sacrum, elbows, and heels. Click here to see examples of
hydrocolloid dressings.
The U.S. Food and Drug Administration has cleared a transfer dressing from Mölnlycke Health Care US
Sample procedure for nonsterile dressing change
By Nancy Morgan, RN, BSN, MBA, WOC, WCC, DWC, OMS
Each month, Apple Bites brings you a tool you can apply in your daily practice.
Description
• Nonsterile dressings protect open wounds from contamination and absorb drainage.
• Clean aseptic technique should be used to change nonsterile dressings.
• In the event of multiple wounds, each wound is considered a separate treatment. (more…)
Foam dressing
By Nancy Morgan, MBA, BSN, RN, WOC, WCC, CWCMS, DWC
Each month, Apple Bites brings you a tool you can apply in your daily practice.
Description
• Semipermeable polyurethane foam dressing
• Nonadherent and nonlinting
• Hydrophobic or waterproof outer layer
• Provides moist wound environment
• Permeable to water vapor but blocks entry of bacteria and contaminants
• Available in various thicknesses with or without adhesive borders
• Available in pads, sheets, and cavity dressings (more…)
Wound Care Meta-Review Draws Firm Conclusions
Wet to Dry
By: Nancy Morgan, RN, BSN, MBA, WOCN, WCC, CWCMS, DWC
In the modern world of wound care, there are many treatment options. Surprisingly though, we are still seeing orders for those dreaded wet-to-dry dressings. Using a wet-to-dry dressing involves placing moist saline gauze onto the wound bed, then allowing it to dry and adhere to the tissue in the wound bed. Once the gauze is dry, the clinician removes the gauze, with force often required. This has to be repeated every 4 to 6 hours. Wet-to-dry dressings are a nonselective debridement method that harms good tissue as well as removes necrotic tissue. It keeps the wound bed at a cool temperature and it at risk for bacterial invasion, as bacteria can penetrate up to 64 layers of gauze! It’s one of the most painful procedures for our patients, and this was one treatment that as a nurse I never wanted to do. In fact, I have heard of nurses who would remoisten the gauze before removal to make the treatment more bearable for patients.
Are you seeing a lot of these dressing still used in current practice? What types of settings are they still being used in consistently? How are you dealing with the prescribing clinicians who continue to order this treatment even though it’s considered a substandard practice for wound care?
Click here to return to Wound Care Swagger
DISCLAIMER: All clinical recommendations are intended to assist with determining the appropriate wound therapy for the patient. Responsibility for final decisions and actions related to care of specific patients shall remain the obligation of the institution, its staff, and the patients’ attending physicians. Nothing in this information shall be deemed to constitute the providing of medical care or the diagnosis of any medical condition. Individuals should contact their healthcare providers for medical-related information.
Read More