By Nancy Morgan, RN, BSN, MBA, WOC, WCC, DWC, OMS
Description
Collagen, the protein that gives the skin its tensile strength, plays a key role
in each phase of wound healing. It attracts cells, such as fibroblasts and keratinocytes, to the wound, which encourages debridement, angiogenesis, and reepithelialization. In addition, collagen provides a natural scaffold or substrate for new tissue growth.
Collagen dressings stimulate new tissue growth and encourage the deposition and organization of newly formed collagen fibers and granulation tissue in the wound bed. These dressings chemically bind to matrix metalloproteinases (MMPs) found in the extracellular fluid of wounds. MMPs normally attackand break down collagen, so it’s thought that wound dressings containing collagen give MMPs an alternative collagen source, leaving the body’s natural collagen available for normal wound healing.
Related Articles
Critical care of the skin – Pressure injury (PI) care bundles help to reduce variations in care and improve outcomes….
Transitioning wound care patients to post-acute care – When discharging a patient who needs wound care, acute-care clinicians (wound care nurse, discharging nurse, and case manager) should…
Wound dehiscence – Dehiscence of abdominal surgical wounds is a medical emergency and requires immediate action to reduce…
Indications
Examples of wounds that may benefit from a collagen dressing include:
• partial- and full-thickness wounds
• wounds with minimal to heavy exudate
• skin grafts and skin donation sites
• second-degree burns
• granulating or necrotic wounds
• chronic nonhealing wounds (to jump-start wounds that are stalled in the inflammatory phase by reducing mediators of inflammation).
Contraindications
Don’t use collagen dressings in the following circumstances:
• third-degree burns
• patient sensitivity to bovine (cattle), porcine (swine), or avian (bird)
products
• wounds covered in dry eschar.
How to apply
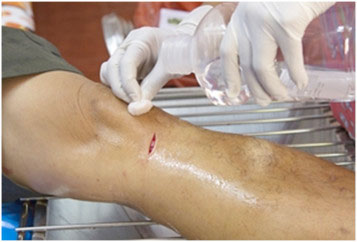 Some collagen products will require a secondary cover dressing. Application technique varies based upon manufacturer recommendations.
Some collagen products will require a secondary cover dressing. Application technique varies based upon manufacturer recommendations.
Frequency of dressing changes
The frequency of dressing changes varies depending on the brand, but ranges from daily to every 7 days.
Formulations
A variety of topical formulations of collagen are available, such as freeze-dried sheets, pastes, pads, powder, and gels. Some dressings include alginates or even antimicrobial additives. The collagen source varies—bovine, porcine, or avian.
Products
Examples
BGC Matrix®; BIOSTEPu Collagen Matrix; Catrix® Wound Dressing; CellerateRX® Gel or Powder; ColActive® Plus; Excellagen®; FIBRACOL® Plus; Promogran Prisma® Matrix; Puracol® Plus; Stimulen™ Collagen Gel, Lotion, Powder, or Sheets; Triple Helix Collagen Dressing
The HCPCS (Healthcare Common Procedure Coding System) codes for collagen dressings are A6021-A6024.
Nancy Morgan, cofounder of the Wound Care Education Institute, combines her expertise as a Certified Wound Care Nurse with an extensive background in wound care education and program development as a nurse entrepreneur. Read her blog, “Wound Care Swagger.”
Information in Apple Bites is courtesy of the Wound Care Education Institute (WCEI), copyright 2013.







I have been struggling to apply Promogran Prisma to a wound that I can’t see, even with mirrors,etc. I don’t understand why I can’t find a therapeutically similar dressing in the form of a paste or gel that would be easier to use. I don’t qualify for homecare as I am not “homebound” Please help.
Hi George I don’t know enough about your wound to advise you what to use. But to talk about collagen generically there are different types of collagen dressings out there. Here is a website that has collagen gel: http://www.celleraterx.com/
I have a patient with a 3 x 3 cm area of hypertrophy with a .5 cm skin break inguinal area, secondary to an intralesional steroid injection. Treatment options are limited. Which collagen product, if any would you recommend?
I have been fighting a diabetic pressure wound on my foot for 2.5 yrs—-my wound specialist has just begun to use collagen on it–does the collagen patch adsorb?—I was told not to remove it, but I cannot find it.
Hi Joanna, most of the collagen products are biodegradable and “dissolve” right into the wound bed. So it is not abnormal for you not to find or see the collagen product you have been using. Hope that helps!
I have got leg ulcers and have sickle cell anaemia, tried many options but nothing seems to be working. It’s been over 3yrs and this is increasingly frustrating. I would like to be guided on direction for use if this gonna work.
P.S can’t even get this product in my country so, I’m hoping to get that arranged too.
Y not try to use dermacyn woundcare solution n hydrogel
Is this not have any side effect on the body. I am allergic to some chemicals. Its is safe to use on all types of external wounds.
@Alvin I can’t say yes it would work…. cause I would need to know more info about your case. In order for a wound to heal you need alot of diff factors to be in place and it would be difficult to determine this. Its not just the dressing you use its everything else-labs/history/meds/nutrition you are on/more details on what the wound is etc etc.
I can understand how frustrating this is to have a wound not heal but the answer is not in just the dressing itself ..its all the other factors that need to be considered. In order to do that I would suggest having your MD or a wound care clinician to do a full comprehensive assessment and identify if this is an option.
Good luck with this Alvin
i have 70 year old with non arterial non venous ulcer in gaiter region looks benign, histology benign, vasculitis negative always looks like a healing wound bus shown no shrinkage in size14x7 cms approx. any topical healing agent you would suggest please
Until you know the cause behind the wound it is really hard to advise treatment. Review the patients co-morbidities, nutritional status and other issues that may impede wound healing and be sure they are addressed.
Maybe start with some referrals to specialists: more vascular studies, a dermatologist referral or even an infection specialist to rule out issues like a change in blood flow, a malignancy or immunological issue, or infectious issue. Start from ground zero, once you are sure the wound has good blood flow, isn’t infected and you aren’t dealing with an unusual type of wound that might require systemic treatment then you might want to consider advanced modalities like a collagen dressing or even things like negative pressure wound therapy, skin substitutes or hyperbaric oxygen therapy to assist with wound closure, but you need to find out the cause of the chronic non-healing ulcer and be sure you have addressed issues like nutrition and any health issues before you can safely apply treatment.
Good luck!
Hi, I have been treating a non healing malleolus wound with hardware at the wound bed from a surgical procedure. Treatment has been with use of collagen and now calcium alginate both changed every 2 days. The wound is getting bigger and more superficial. It was positive for pseudomonas. Any suggestions?
Hi Karrie,
Something doesn’t sound right here… This is an acute wound so it should be getting smaller not bigger… My first question was did you treat the wound topically for the Pseudomonas? Start back at ground zero with your comprehensive wound assessment, you may still be dealing with infection here, I would re-evaluate and be sure if you are seeing s/s of infection you treat it topically with the appropriate product on the wound bed to target the bacteria. Be sure the wound bed is getting adequate blood flow as well.
I don’t know much about the patient or wound bed here, but an acute surgical wound should heal up, if not it might be stuck and need some help, start back at ground zero with your full assessment. Remember to practice warm moist wound healing principles and look for s/s of infection, consider an hardware issue – is the patient having increased pain? Reach out to the surgeon if you need to.
A good assessment will help give you the answers you are looking for 🙂
Good luck!
At my facility we do not have a collagen gel product. I have a pt that has a stage IV PU without any slough. The wound bed is clean. Drainage is scant. So, I thought collagen would be helpful. The only issue is that the wound does not have any tunneling, but the depth is 2cm. So, I feel like I need a filler along with the collagen product (Puracol plus). Is there any problem with using the Puracol and a gel like Saf-Gel to fill in after the Puracol is layed on the wound bed?
Hi Sandy,
You are always going to want to refer back to the package insert to be sure your secondary dressing is appropriate,and safe to use. Often our secondary dressing even when using a collagen is based on the amount of exudate. I would advise reaching out to your product vendor for advice on how to use this product the best way for your patient and still being cost effective for your facility to get your patient the best healing outcome possible 🙂
Good morning… I have this 23year old lady with full thickness burns TBSA about 54% (both lower limbs and uper limbs, face and chest)…. how often do I need to be doing the wound dressing and debridement …. and will she benefit from collagen gel?
Hi,
I am not sure what setting you are caring for this patient in but per the American Burn Association it is recommended that anyone with full thickness burns that cover greater than 5% of their body surface area are transferred to a burn unit for specialized care. Typically debridement and topical antibiotic therapy are needed here with the specialized care in the burn unit, collagens aren’t indicated at this time during the acute management of the burn patient. Debridement of eschar and management of infection is priority. Good luck!
why not for 3rd degree burns?
Hi Maria,
Burns need to be handled in a very special, they require ongoing management of topical infection and debridement necrotic tissue before using various products on them. Often skin grafting is involved here too.
There are just not enough studies to back up and to support using many topical dressings on the full thickness burn patient; collagens are one of them.
On the collagen dressing package insert, you will see that it is “contraindicated” for use on third degree burns and we need to apply dressings as indicated per our package insert.
I have been doing wound care for my sister every day since May. Her wounds appear in her creases, below breast, in the groin, below belly overhang. She knows that weight loss is very important to the cure but in the meantime we have these nasty wounds to care for. The bad ones are about 1 cm deep at the deepest and have been up to 5 cm long. It took 3 months to get one really bad one finally healed. Yesterday she asked if I wanted to try the collagen the wound care doctor gave her and I think it’s a good idea, but am unsure how to use it. The product is little tiny flakes. Do I just shake it into the wound and then cover it or put a gel on top of it. Then how often do I clean the wound if at all, (still having some yellow/brown exudation). Help!
Hi Valerie, the best thing to do is read or obtain the product insert. Many times you can find it online if you google the product name. I would obtain the product insert and follow those directions. Each product is diff so it would be difficult for me to advise you. Sound like you are doing a good job with your sister! Keep up the good work!
Nancy
hi Nancy: Very well written. One additional section would have made it more comprehensive is about the mode of action of collagen once applied (both from a chemokine perspective, where collagen attracts inflammatory cells to the wound bed and its potential to act as a substrate to excessively produced interstitial collagenases to kick-start the “protection cascade” of intrinsic collagen. From my experience, this is one point I have that distinguishes different brands in terms of efficacy.
Anyways thanks for providing a very good insight.
Thanks Dr Anil, yes I hear you… I could add more and actually this is one of my fav topics cause Collagen can really accelerate healing. I focused on this just being a quick guideline tool. I appreciate your feedback!
Treating a small ulcerated and doctor debrided area between little toe and adjoining. Third day of treatment. Margins appear pinkish, is that okay? Also was told to pack Prisma, a very small piece, into the wound to make sure it adheres. Should any of it extend to the surrounding margins?
Hi! is it good for st4? its in lateral malleolus. it has min exudate.
Hi Jamille you will need the kind that is in a gel form because you don’t ahve much drainage. Here is a link to a product that will be helpful:
http://www.elastogel.com/product-catalog/wound-care/stimulen-collagen-wound-care#st9505-stimulen™-1-oz-amorphous-gel-tube
are u suspose to pack deep tunneling wounds that have been debreeded with prizma or just put it over the out hole
Teresa,
If you are talking about Promogran Prisma dressing, then the dressing needs to touch the wound bed. Promogran dressing can be cut to size and is absorbed into the wound, so no need to remove. Here is link for more detailed information: http://www.systagenix.net/our-products/lets-promote/promogranandtrade-186/indications
Nice Articel
hi! can i use collagen to stage 4 PU ON ISCHIUM?
I would like to know what is the best way to apply purcol (collgen) to a round wound in my stomach.
I have looked for examples and can’t seem to find any. The round wound comes from a second infection after I had hysterectomy. It is right in the center of my incision. First used gauze with dakins( 1/2 gauze) changed twice daily. Also used rolled gauze with dakins on main or first incision.
Went to wound Physician and he changed my dressing to purcol. Would like advice on how to fill hole with this new collgen. Thank You
My husband is diabetic and got cellulitis on all toes on one foot a year ago. Today he ended up with a blister on his heel from the inside sole of his shoe coming apart and the seam part rubbing it, he thought it was something in his shoe. I still have some of the puracol plus ag left from last year, would I be jumping the gun if I went ahead and put a little of it on the part of the blister that busted? I have the Puracol Plus AG pad type thing.
Just wanted to know your thoughts about the application of TheraHoney gel on heel pressure ulcers ? in general. Thanks much, Lydia
excellent for curing wounds.I used it healed myself.
I got a wound on my leg and I’ve done scan and wound swap the result said it’s clostridium difficile want to know which of the collagen products is best to help heal the wound