By Nancy Morgan, RN, BSN, MBA, WOC, WCC, DWC, OMS
Each month, Apple Bites brings you a tool you can apply in your daily practice.
Description
A hydrocolloid dressing is a wafer type of dressing that contains gel-forming agents in an adhesive compound laminated onto a flexible, water-resistant outer layer. Some formulations contain an alginate to increase absorption capabilities. The wafers are self-adhering and available with or without an adhesive border and in various thicknesses and precut shapes for such body areas as the sacrum, elbows, and heels. Click here to see examples of
hydrocolloid dressings.
Actions
Hydrocolloid dressings are occlusive, so they provide:
• a moist healing environment
• autolytic debridement
• insulation.
Advantages
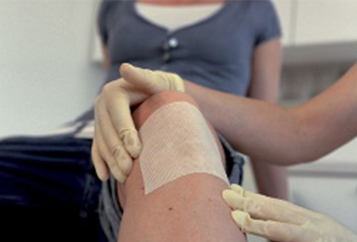 • Impermeable to bacteria and other contaminants
• Impermeable to bacteria and other contaminants
• Self-adherent and mold well (don’t adhere to the wound, only to the intact skin around the wound)
• May be used under venous compression products
• Easy to apply
• Minimally disrupt healing (the dressing can be worn for several days before it needs to be changed. See “Frequency of dressing changes” for more information.)
Disadvantages
• Not recommended for wounds with heavy exudate, sinus tracts, or when infection is present
• Must be used with caution on the feet of patients with diabetes. It’s suggested that hydrocolloid dressings can be used safely on diabetic foot ulcers if 1) they are used only on appropriate wounds after a thorough patient assessment, 2) the wound is superficial with no signs of infection, 3) there is low to moderate exudate, 4) there are no signs or symptoms of ischemia, and 5) dressings are changed frequently
• Assessment can be difficult if the hydrocolloid dressing is opaque
• May become dislodged if the wound produces heavy exudate
• May curl or roll at the edges
• Upon removal, dressing residue may adhere to the wound bed and there may be an odor
• May cause periwound maceration (see photo)
• May cause trauma/injury to fragile skin upon removal
• May cause hypergranulation
Related Articles
A guide for adhesive removal: Principles, practice, and products – Improve your knowledge on how to remove medical tape or wound dressings….
Moisture-associated skin damage: The basics – Moisture-associated skin damage (MASD), inflammation and erosion of the skin, results from prolonged…
Wound dehiscence – Dehiscence of abdominal surgical wounds is a medical emergency and requires immediate action to reduce…
When to use
A hydrocolloid dressing is appropriate for these situations:
• noninfected wound with scant to moderate drainage
• necrotic or granular wound
• dry wound
• partial- or full-thickness wound
• protection of intact skin or a newly healed wound.
Frequency of dressing changes
• Change the dressing every 3 to 7 days depending upon exudate and manufacturer guidelines.
• If daily dressing changes are required, reconsider the appropriateness of this approach because these dressings are designed for extended wear for up to
7 days.
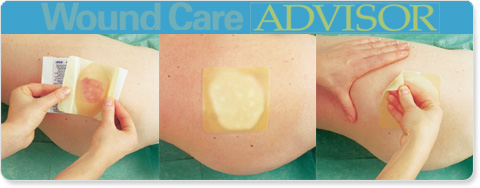
How to apply a hydrocolloid dressing
1 Wash your hands and put on gloves.
2 Remove the soiled dressing (noting the date it was applied) and place it in a trash bag.
3 Remove your gloves, wash your hands, and put on new gloves.
4 Clean the wound with normal saline
solution or prescribed cleanser.
5 Use clean gauze to pat dry the tissue surrounding the wound.
6 Remove your gloves, wash your hands, and put on new gloves.
7 Apply liquid barrier film or moisture barrier to the periwound area.
8 For deep wounds, apply wound filler or packing materials as indicated.
9 Before applying the hydrocolloid dressing, warm it by holding it between your hands to increase adhesive ability.
10 Remove the paper backing from the dressing.
11 Gently fold the dressing in half lengthwise and apply it from the center of the wound outward.
12 Smooth the dressing in place from the center outward. Hold the dressing in place for a few seconds to improve
adhesion.
13 The dressing should be at least 1 inch larger than the wound. (Some manufacturers may require a 2-inch border.)
14 You may apply tape around the edges to secure the dressing.
15 Dispose of the waste.
16 Remove your gloves and discard.
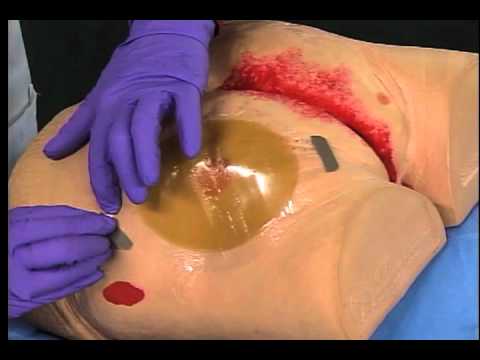
 How to remove a hydrocolloid dressing
How to remove a hydrocolloid dressing
1 Press down on the skin and carefully lift an edge of the dressing. Continue lifting around the dressing until all adhesive edges are free.
2 Gently peel away the dressing from
the skin in the direction of the hair growth.
Selected references
European Pressure Ulcer Advisory Panel and National Pressure Ulcer Advisory Panel. Treatment of pressure ulcers: Quick reference guide. Washington, DC: National Pressure Ulcer Advisory Panel; 2009.
Hess CT (ed). Clinical Guide to Wound Care. 7th ed. Philadelphia, PA: Lippincott Williams & Wilkins; 2012.
Nancy Morgan, cofounder of the Wound Care Education Institute, combines her expertise as a Certified Wound Care Nurse with an extensive background in wound care education and program development as a nurse entrepreneur.
Learn more about wound care at the blog “Wound Care Swagger.”
Information in Apple Bites is courtesy of the Wound Care Education Institute (WCEI), copyright 2013.







I have been given these extra thin dressings for an open wound in the corner between nose and cheek after MOHs op just one slice took but still about 1/4” deep about the opening size of a nostril. I was told I would need to change it every two days but it’s now a week since and still have to change it at least twice a day because it fills up with fluid and the eventually leaks. It’s not infected. I go back hospital end of this month
Harry. I have the same problem from MOHS surgery. What dressing did u use or switch to and what worked.
Hi Harry,
If you are using an extra thin hydrocolloid dressing, these aren’t made to typically handle a lot of wound exudate and are made to be left in place for extended period of time, some 5 days depending on the manufacturer. If you are changing the dressing multiple times a day, it might not be the right dressing for you, I would check back with your prescribing clinician and let them know about the drainage amount to be just to be sure…
Good luck!
Nancy WCEI
Hello: I have developed a pressure wound on the bridge of my nose from wearing a Bipap mask. Which thickness and brand of dressing would you recommend?
Hi Elaine,
The type of dressing really will depend on the amount of drainage you have. You don’t want anything to bulky as that will alter the seal of the face mask of your Bi-pap. A thin silicone foam dressing may be a good place to start, again this will be depending on the depth of the wound, signs of infection, and exudate level. Dressings can help, but ultimately they won’t fix the problem. The pressure from the tightness of the face mask. Be sure that you have the right “fit” for the mask. You might want to consider a “gel” pad after your wound has healed up to prevent further breakdown. Always, whatever you do, be sure to check with your physician in regards to an open wound if it is not improving or has s/s of infection such as redness, warmth, increasing pain, odor or drainage. Good luck!
Nancy WCEI
My mum keeps getting infections around her stoma. I have heard she can place a hydrocolloid dressing on, before sticking the bag back on. Is this a workable solution and do you recommend this? Will she need to cut a hole in the centre of a dressing, or are there some that are wound specific such as for a stoma? It is in the centre of her stomach.
Hi, Nancy:
I Took a nice thick slice off upper portion of thumb with a mandolin slicer on Monday. it’s now Sunday.ER doc applied duoderm to adhere flap back in place. didnt change dressing for 4 days. change daily now. itchy today. should i force duoderm off or let it fall off?
Hi Linda, first and foremost if she is getting “infections” you need to find out what type of infection present before using hydrocolloid because this product is a occlusive dressing meaning it would trapped bacteria underneath it and “could” cause a super infection. So to be safe identify what type of infection. Once you know that you can re post and let me know. Thanks, NancyWCEI
Hi Rita, this product can be left in place 3-7 days. Am I reading right ?….you are now changing this daily if so, that is too often this product is meant to stay on for an extended period of time and the adhesive backing is strong and by pulling it off every day could hurt the skin and flap. Make sure you don’ t have signs of infection-redness/increased drainage, swelling etc. If no signs of infection ok to use hydrocolloid make sure you size it about 1 inch larger then your wound as you want it to adhere and seal down on all sides.
Good luck with this. NancyWCEI
Hi Nancy. I am a home health nurse. I am treating a patient for a wound to Right BKA site, it’s got some dry, thick flaky skin and a small open area, 2.5 cm x 0.5 cm. I am thinking hydrocolloid three times a week will do the trick because it will add some protection to the area. Her prosthetic tech says she can still wear the prosthesis just not for prolonged periods until the wound heals. What do you think?
Hi to RN4life-if there is depth to the open area dead space should be filled prior to hydrocolloid placed on top of it.
I would be careful on using this product in that area for a few reasons -becareful on removal if not done properly could tear the site open more. Make sure there is no infection present if you use this, cause this is occlusive drsg and could create a super infection. You might even can consider changing 1-2x per wk if things are going ok and the product insert states that frequency is appropriate . Also make sure you size this drsg larger than the wound by min 1 inch so you have plenty of anchoring area to adhere to the skin. If you can, use a “beveled” edge hydrocolloid product (where edges are thinner and more flexible) this will help decrease the rolling on the edges and melt down and adhere better to the skin. Hope that helps !
My hands were steam burned on June 30, 2013. They were deep 2nd degree, almost 3rd degree burns. I did whirlpool and physical therapy. I used LOTS of silvadene. I never got an infection. My hands look wonderful (no scarring, no wounds) but it’s obvious that I do not have all layers of skin. Is there a product I can use to help regrow layers? I am an RN and am not working as the gloves stick to my hands, and handwashing is extremely irritating, plus I feel like I have raw nerves that cause worse pain when I do much with my hands. Any ideas?
Hi Nancy,
I am considering a hydro colloid on a tricky wound I am treating in my practice. My lady lacerated her shin whilst getting out of a car, she is mid 70s, ER stitched the wound approx 6 inches long. sutures are now out. The wound is a large C -shape and the inside of the ‘C’ is very hard and black. Would a hydrocolloid be a good choice to help debride and create a moist environment. looks like a hematoma had developed under the wound in the initial stages after suturing.
Hi Katie, you could try it if there is no s/s of infection and its not draining much.
OR if there is some drainage you can consider a foam dressing that would give it some extra insulation and padding.
Amy if you had a 3rd degree burn that means its full thickness–means you have burned thru the layers of the skin – epidermis and the dermis. The dermis is where nerves are located. When the site heals it will heal with granulation tissue and then the epithelial cells will migrate across the wound bed to closure.
There is nothing that will bring back the dermis layer back.
I would consider a good moisturizer to be used all the time.
Also check out the type of gloves you have there are diff grades of gloves and the nitrile gloves do stick anyone’s hands even tho they are tougher and no latex, they are also 3 times resistance to punctures. Your facility may of chose this type of gloves for these purposes but perhaps you can test drive a diff type.
Good luck with this
Hi Nancy,
I have a wound in the crease of my leg. Doc said to use DuoDerm. the patch stays on for a 2 days at most and that’s if I put some gauze on the wound to help catch the goopy stuff. The would only seems to drain a lot when the duoderm is on it. after reading other posts, i’m thinking this isn’t the right bandaging approach and want to know if you have some suggestions. i’m using the 4×4 duoderm. is it ok to put gauze under the duoderm patch? thanks
Hi Joyce, I am thinking if you are seeing a lot of drainage this isn’t the right dressing for your wound, hydrocolloids aren’t designed to hold a lot of exudate or drainage. Depending on how deep your wound is you may need to lightly pack the wound with an alginate or hydrofiber and then apply the hydrocolloid. I would reach out to your prescribing clinician and talk to them about the amount of drainage and the dressing prescribed, and to be sure the wound doesn’t need any further assessment. Good luck!
Dr. Says I have Venus stasis ulcer. Started duoderm today. What do you think. On anterior lower shin.
Hi Kathy,
As long as the Duoderm holds/absorbs the drainage from the wound and doesn’t keep the surrounding skin to wet it should be fine 🙂 the important thing with venous ulcers is to treat the underlying cause – to get that “fluid” back up toward the heart; and that is usually done by some type of compression. As long as you have good arterial blood flow in your lower extremities, the standard of care is to wear compression wraps or stockings to treat this Venous Hypertension which is what causes these venous stasis ulcers otherwise they don’t heal, and just keep coming back! If the Duoderm doesn’t soak up the drainage, sometimes patients need a dressing that soaks up/absorbs more drainage like a foam dressing, and that can be used under compression wraps as well. Good luck!
Hi, my father has developed a pressure sore on his paralyzed thigh, and its getting bigger with an wound about half inch in diameter and 1-2 mm deep. it oozes some exudate. what type of duoderm dressing should i use? could u tell me the applying instructions? and how often should i change it? kindly reply. thanks.
Hi Naz,
There are different types of hydrocolloids on the market, Duoderm and Exuderm are brand names for example. You want to be sure the dressing is 1-2″ larger than the wound. As far as general application refer to the section above called “How to apply a Hydrocolloid dressing” but always follow the specific products package instructions. A key point here is to always offload the wound or “sore”, meaning to try to have as little pressure on the area as possible. Since the area on your Dad’s leg is getting worse, draining exudate, and has some depth to it a hydrocolliod might not be the best choice as it will not fill the depth of the wound bed. It would be a good idea to have the wound evaluated by a certified wound care clinician or his primary healthcare professional at this time. Good luck!
Hi, I wonder if you can clarify something for me about hydrocolloid dressings. I had two very small wounds following a hip arthroscopy which were healing very well; completely dry and no sign of infection. Plasters I had on were coming off so I wanted to replace them for just a few days more. I chose a hydrocolloid dressing from a supermarket primarily because they were bigger than a normal strip plaster. When I took the plasters off about 5 days later they removed my scabs. I now have unsightly scars because the scabs didn’t come off naturally. Should this happen? I would appreciate hearing your view. Many thanks. Rachel
Hi Rachel,
I have to say first that I am unfamiliar of what you mean by “Plasters” I am assuming this is a post op dressing /bandage and not some type of device or pinning (maybe you are not from with in the united states and plasters is a term from your location?) So as long as this was a bandage over the surgical incision, we can continue on, as I understand it is the type of surgical dressing you had in place. Healing and scar formation of a surgical incision depends on several factors including how the surgeon closed the incisions, did they use sutures, staples, skin glue/adhesive or was the incision left open to heal from the bottom of the wound up.
You didn’t mention surgical wound closure but you did mention a “scab” so I am going to guess (but I might be wrong) that these incisions were left open to heal from the bottom up, and the way a full thickness wound heals by scar formation, the scar will be more noticeable when we do not re-approximate or bring together the edges and secure them with sutures, staples or skin adhesives.
So really it is not that your dressing selection was incorrect, or your wound got worse, it most likely was that under that scab there was still a lot of work the wound had to do to fill in with granulation tissue (scar tissue) to fill in to get up to the top of the wound bed where it then could resurface with new epithelium. It might just not be done healing yet.
The best thing for a wound is to manage the drainage (if any) keep it warm and promote moist healing while keeping it free of infection. Any further questions or signs of infection I would refer back to your surgeon. Good luck!
Hi I’m just wondering how long a waterproof dressing can be left on for when there’s some ooze that’s a little smelly? My dad’s 80 he had a fight fermol bypass couldn’t use vein used graft that blocked appox 6 weeks post surgery limited blood suply keeping the leg and foot alive he has 2 abscess’s on his leg above knee that continually ooze nurse dress’s once a week and my mam if it needs be before nurse calls he’s on long term antibiotics but today nurse called changed dressing and said it should be left until next week until he sees consultant but that’s 6 days away my worry that she said it’s smelly and from past issues infection has spread quite quickly and docs will not remove graft as what do they put in its place? And with being 80 with asthma another surgery is totally unadvisable? So should dressing be changed sooner that 6 days? I know to watch for further signs of infection as in temp redness pain in foot or coldness or really hot to touch we’ve being on this roller coaster for 4 years!!
OK I have a venous stasis ulcer an I was using douderm but it was constant ly oozing an I wore for three weeks I all the sudden developed a sever allergic reaction so they s after me on perdnisone an I finished script the hives are back and it feels like the skin around it is burning so the put me back on more prednison an it still hurts solo bad the sore is on the inside of my ankle but my shin bone is so sore what do think is going on I have also used silvadine please PLEASE HELP IN TERRIBLE PAIN AN HAVE BEEN TO DOC AN SPECIALIST
@Brandi a few things duoderm should not be used for 3 wks that is too long and it really don’t absorb that much drainage. Due to the allergic reaction I would stop the use of duoderm immediately.
If this is truly a venous ulcer consider using a foam dressing or alginate or if there are large amt of drainge go into a hydrofiber or specity absorptive. Also some form of compression wrap or stockings should be in place to help with this.
Hi I had a feeding tube removed 1 month ago and while the wound has stopped leaking there is still a large hole. I have duoderm left over from a previous abscess and would like to know if I can use duoderm on my feeding tube site to fill in the hole. Thanks
Hi Nicole,
I wouldn’t use the Duoderm, a better choice would be a foam product.
Good luck!
mole biopsy, groin area (curve of glute, near inner thigh) smaller than a nickel, I think. I live alone and I can either see the area or reach the area, but not both at once and I really can’t see it all that well.
I was given an anti-bac cream, told to keep the wound covered with that plus “any bandage” for 2 to 3 weeks, change daily. Based on what I am reading here, I think a foam bandage might be a good choice because of the need to change every day? Thank you for work work on this website!
Hi Lee,
Actually, if you need to change the dressing everyday a Composite Dressing might be a better choice as the foam dressing is meant to be left in place for long periods of time as well. The composite has multiple functions and has 2 products that are manufactured into one bandage; for example,an absorbent pad with an waterproof outer adhesive covering. The outer covering is impermeable to bacteria as well. These are used frequently in our post op patients. Good luck!
My mom who is wheelchair and bedbound has developed a pressure ulcer on her rt.cocyxx. She has stage 2 wound and the home health nurse put a thin duoderm
dressing. The edge keep sliding exposing part of the wound. No signs of infection or not much exudation. Can we also use duoderm border to avoid peeling off easily but worried abt. the skin tear if I peel off during dressing change since it sticks really good. Would it help if I put no sting barrier around to avoid skin tear?
Hi Edna,
You could use the Duoderm border dressing that might help. Applying no sting skin sealant or skin prep around the area before applying the Duoderm will help protect the skin when removing the Duoderm as well. When removing the Duoderm, gently lift an edge and then continue to lift all the edges all the way around before gently peeling the dressing back. When repositioning your Mom in bed and in chair be sure to lift her completely and avoid sliding her which may be contributing to the dislodging of the Duoderm as well. Use draw sheets or lift sheets etc. Ask your home health team for ideas.
Good luck!
Hi Nancy,
I am an RN about 5 weeks postop. This past November I had emergency surgery for a perforated bowel and had a temporary colostomy. This latest surgery was total sigmoid resection with colostomy closure. I have a vertical incision up past my umbilicus which was reopened for the colostomy takedown. I also have a smaller transverse incision to close the ostomy site. Could you please suggest a product that may help to decrease the formation of scar tissue and flatten the scar. I have been using “Scarguard ScarSheet MD(Silicone Scar sheets),but I find they do not adhere to the skin without covering them with Mefix tape. This is changed up to Q48 hours. I have read that a hydrocolloid product ( Duoderm Extra Thin CGF) works well in decreasing scar and can be changed Q3 to 7 days if there is no exudate. I have also heard that applying paper tape and changing prn can also help. The silicone also comes in a paint on liquid that you apply BID.My incision is well healed, edges well approximated and no drainage. I have started massaging the incisional area as well. Could you please give me your thoughts and suggestions on the above matter!
Look forward to hearing from you soon!!!
Hi Nancy, any response to my post to you on April 28th? I have delayed any thoughts in dressings or treatment to my incision until I heard from you. Cheryl
Hi..
I have my breast abscess removed early February which left me with a huge and deep open wound. The wound is healing fast, which now is only small and superficial. I used Aquacell Ag before but now only use duoderm. My problem is duoderm seems to cause my wound to produce a lot of gooey stuff. I couldnt use gauze of plaster since my wound will only stick to the material. I change the dressing twice a day. Should i go back to using aquacell? The problem with aquacell now is that the material tends to dry and sticks to the wound and makes it difficult to change the dressing.
Hi, sounds like you need a different dressing for your healing breast abscess removal. The Duoderm is not very absorbent and shouldn’t be changed so frequently, and the Aquacel you were using is meant to absorb heavy amounts. Maybe a better dressing selection would be a thin foam dressing that will absorb some of the drainage you are having and will be non-adherent to the wound so it won’t stick. The foam dressing is meant to be left in place for longer period of time depending on your drainage level you can change it when you see the drainage outline on the back of the dressing, usually day 3-5. Another choice would be the composite dressing where there are 2 products manufactured into 1 dressing, so you have a non-adherent absorbent pad with an adhesive border around it. This would be appropriate as well. With the healing abscess we don’t want any “occlusive” dressing like the Duoderm usually as we want the pus (material left inside) to be able to escape and drain. This is why you may have seen more “gooey” drainage. Good luck!
Nancy, my daughter has fallen on her bottom when riding a little scooter. She has a scrape about 4×8 cm. it looks like awhile layer of skin came off without much bleeding (like was blister looks like if you took the ‘bubble off’. Would you recommend hydrocolloid dressing? I’m worried with sitting and normal activity traditional bandages would stick to the wound, come off or let urine soak in (she’s 5).
@Tammy – Sorry to hear about this, from the limited information provided here I agree that a thin hydrocolloid dressing may work well. It will trap in moisture which is needed for healing at the same time blocking outside contaminates like urine from entering. If there are signs of infection – redness, swelling, pain, pus or lots of drainage, this would not be my recommendation. Other options include the use of transparent dressings, which are waterproof and some cover type dressings as well.
Hi Nancy still waiting for a response to my questions to you dated April 28.
Hi, my 6 yr old daughter fell an got rug burn pretty bad on her face. Right around and on one side of her nose and nostril. I’m not sure if there is an appropriate type of bandage to put on it – I’m worried about infection because it goes under her nostril and I also want to avoid scarring. I’ve been trying to keep it moist with antibiotic ointment, but it does already seem to be forming a scab. Any advice would be appreciated. Thank you!
Hi..whats different between the dressing and the paste and the gel? My baby got broken skin near the bottom area due to the nappy rash. It’s been 3 weeks. My plastic suggest to use dressing. But it is on the difficult area. Can not get the gel. Only have the paste. Please advice the different between those. Thank you
@Adriana – its hard to advise on the web I would need more info. but……keep looking for the signs of infection and consult your MD for advise.
@Merlyn-babies can have lots of diff rashes I would figure out the root cause of this rash with MD and whatever you end up using “make sure” its for babies many of the current wound care products out on the market is not for babies.
Nancy did I not ask an appropriate question regarding postop wound care? I am an RN but do not pretend to know everything.That is why I emailed you for suggestions. Thank you.
Hi please could you tell me what the dressing are made of? I have been told that a non-woven viscose product is similar to wound care products and I wondered if this is true.
Thanks
Hi Sue, it contains a combo of sodium carboxymethylcellulose, pectin .
Gel forming type material that can be connected to a semi-permeable film or foam backing.
Brand name example-Duoderm
Hi Nancy, An elderly relative’s best current option for urinary incontinence is to use an external petal catheter with hydrocolloidal adhesive, such as the ReliaFit or Men’s Liberty products, but he is afraid of tearing the perfectly normal but delicate/sensitive skin of the glans, upon removal of the adhesive. I notice that you list possible damage to delicate skin as a disadvantage of these adhesives. But is this a realistic reason to avoid such adhesive for normal skin of the glans? With plenty of care during removal (very slow peeling, soaking the bandage’s peeled edge, etc.), is damage a large or small, serious or minor, risk? All other options that permit independent living seem not to have worked out. Thank you for any advice!
Art this is a consideration on the list based on indiv patient situation. It does not necessarily mean to stay away from everything on the list. Just to take precaution.
Reliafit looks like on the video may have a adhesive removal item (that is not part of the kit) this might be worth investigating as well to avoid skin breakdown
http://www.eloquesthealthcare.com/reliafit/#
I have HS and am wondering at what stage should I NOT be using this type of dressing. I am currently draining and am not sure but would love the relief it gives right now. Thank you in advance!
Hi just to clarify what is a HS?
Hi Nancy,
I used to have an abscess in the right buttock just about 1 in away from the right hip bone. It was for about 4 years, opened in its own right, and being drained, then it was self-closed, then it was re-open to drain, etc. I used to put a gauze and taped it every once in a while, until 1 month ago, I’ve seen a surgeon in ER and he drained it well, squeeze it, put a pack. The process was continued for two more days. After a week, I didn’t feel much pain in the abscess but the pain was very close to the right hip bone (about 0.5 cm away), I asked the same surgeon who cleansed the abscess, he told me this causes some necrosis because of the pressure. He advised to both lessen my sitting down, and to use a special cushion adhesive. An ER nurse suggested me to use the ConvaTec DuoDERM extra thin CGF dressing. I just applied it, and it works as magic, no more pain in the hip’s bone.
Does it really over the 4-year period abscess I developed the skin pressure ulcer? Is this DuoDERM will heel the ulcer or do I need to seek more medical advise?
Thank you Nancy.
Hazens this is hard to give you my opinion cause I don’t know enough on this case and I can’t see it. However I have seen this “opening and closing ” going on alot with abscesses. And they are challenging wounds no doubt. Just when you think its all good…….then it reopens. Pressure can complicate things yes……but I won’t “label” it as a “pressure ulcer” because the cause of this was a abscess. And you now have “complications” from this where decreasing “pressure” to the site is helpful for the healing process. If there is depth to this site the depth would need to be packed and then the site covered. So if you using duoderm and you have depth in the wound you need to fill the dead space (depth) with a packing type dressing then cover the wound. Continue to be monitored by your doctor to make sure no more complications happen.
Good luck with this Hazens!
I have a open leg wound approx 8″ in length & 3″ wide it is just over 12mth old could you suggest a dressing such as DUODERM or AQUACEL to dress it as the leg needs to breathe ive been using a elastic bandage on it for the last 12mth the wound has shrunk considerably in 12mth the wound is about 3mm deep would it need a filling thanx
Rod,
Unfortunately without seeing your wound, we cannot give you directions on specific treatment. I encourage you to contact your healthcare provider for detailed instructions.
Some wound products such as foam dressings and hydrocolloids swell and expand when moist and therefore do not always need additional packing.
Good luck with healing.
Can you use hydro colloid dressings on boils
Diane I would not recommend using this product on boils. I would consult with your MD on treating the boil.
Nancy, my father has been bedridden for almost 2 years. He is unable to communicate or do anything for himself. Although he has been getting great care he has developed pressure wound on his sacral area. It has at times, broken through with mild bleeding but currently is just swollen and purple red in color. Are the thin hydrocolloid wound bandages appropriate to use to prevent trauma to area when he is moved in the bed and will they help in preventing progression of the pressure wound?
thank you
Hi Liz,
Hydrocolloid can be in place if the wound bed is flush with the wound edges (not deep)it would help decrease friction to the site. However if there are any signs of infection which there might be based on your comment that its swollen and bleeding, I would not use this product unless you know there is no infection.
The purple red color concerns me I would make sure he has a special bed (low airloss or alternating air) and also a chair cushion in place.
An option for a dressing to consider would be a foam dressing get it about 1-2 inches larger then the area and that will help insulate it and protect it from friction and its a dressing that you can leave in place for an extended period of time. Allevyn is a brand name of one here is a link: http://www.smith-nephew.com/key-products/advanced-wound-management/allevyn/allevyn-adhesive/
I would off load any pressure to the site to allow this area to heal.
Definitely consult with your primary MD as its hard to advise you with not seeing the wound myself.
Nancy
DISCLAIMER: All clinical recommendations are intended to assist with determining the appropriate wound therapy for the patient. Responsibility for final decisions and actions related to care of specific patients shall remain the obligation of the institution, its staff, and the patients’ attending physicians. Nothing in this consultation shall be deemed to constitute the providing of medical care or the diagnosis of any medical condition.
Can Aquacel Extra be used over Adaptic Non Adherent Dressing for a wound with heavy exuding? With Aquacel Extra and ExuDry secondary dressing there is sever strike through onto macerated skin. If Aquacel could be used over Adaptic it would provide for easier dressing changes an less pain. Before Aquacel we were just using Adaptic with Gentamicin and an ExuDry cover.
I have an apparently uninfected wound . (never cultured). I am retired RN-some wound care knowledge. Not sure about my PA provder. Given these instructions :
Karen reviewed the pictures and feels that the healing is going okay. She understands that you feel it has been very slow going, but she would like you to continue the duoderm, BUT add exposing the wound site to air for an hour or so a couple times daily. Follow up with pictures in 7-10 days. Thank you.
i think these are opposing instructions. what is my best response to her?
Hi Nancy:
I used it on my cat so he doesn’t lick his wound. Now it is almost healed but the gel residue also got stuck with his hair. What would be the best solution for cleaning it from his hair?