Apple Bites
Each month, Apple Bites brings you a tool you can apply in your daily practice.
-
 General characteristics Document if the diversion is an intestinal or urinary ostomy, whether it’s temporary or permanent, and the location— abdominal quadrant, skin fold, umbilicus. (See Descriptor reference.) Describe the type of ostomy: • colostomy (colon)—sigmoid or descending colostomy, transverse colostomy, loop colostomy, ascending colostomy • ileostomy (small bowel)—ileoanal reservoir (J-pouch), continent ileostomy (Kock pouch) •… Read more…
General characteristics Document if the diversion is an intestinal or urinary ostomy, whether it’s temporary or permanent, and the location— abdominal quadrant, skin fold, umbilicus. (See Descriptor reference.) Describe the type of ostomy: • colostomy (colon)—sigmoid or descending colostomy, transverse colostomy, loop colostomy, ascending colostomy • ileostomy (small bowel)—ileoanal reservoir (J-pouch), continent ileostomy (Kock pouch) •… Read more… -
Assessing footwear in patients with diabetes
 Inappropriate footwear is the most common source of trauma in patients with diabetes. Frequent and proper assessment of appropriate footwear is essential for protecting the diabetic foot from ulceration. Here is a step-by-step process for evaluating footwear. Be sure to evaluate footwear with the patient walking, standing, and sitting. Observe wear patterns for areas of high pressure or abnormalities • Check the inside of… Read more…
Inappropriate footwear is the most common source of trauma in patients with diabetes. Frequent and proper assessment of appropriate footwear is essential for protecting the diabetic foot from ulceration. Here is a step-by-step process for evaluating footwear. Be sure to evaluate footwear with the patient walking, standing, and sitting. Observe wear patterns for areas of high pressure or abnormalities • Check the inside of… Read more… -
Causes, prevention, and treatment of epibole
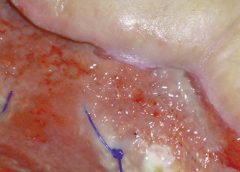 As full-thickness wounds heal, they begin to fill in from the bottom upward with granulation tissue. At the same time, wound edges contract and pull together, with movement of epithelial tissue toward the center of the wound (contraction). These epithelial cells, arising from either the wound margins or residual dermal epithelial appendages within the wound bed, begin to migrate in leapfrog or train fashion across the… Read more…
As full-thickness wounds heal, they begin to fill in from the bottom upward with granulation tissue. At the same time, wound edges contract and pull together, with movement of epithelial tissue toward the center of the wound (contraction). These epithelial cells, arising from either the wound margins or residual dermal epithelial appendages within the wound bed, begin to migrate in leapfrog or train fashion across the… Read more… -
 Topical application of silver nitrate is often used in wound care to help remove and debride hypergranulation tissue or calloused rolled edges in wounds or ulcerations. It’s also an effective agent to cauterize bleeding in wounds. Silver nitrate is a highly caustic material, so it must be used with caution to prevent damage to healthy tissues. Application method Silver nitrate applicators are firm… Read more…
Topical application of silver nitrate is often used in wound care to help remove and debride hypergranulation tissue or calloused rolled edges in wounds or ulcerations. It’s also an effective agent to cauterize bleeding in wounds. Silver nitrate is a highly caustic material, so it must be used with caution to prevent damage to healthy tissues. Application method Silver nitrate applicators are firm… Read more… -
 Each issue, Apple Bites brings you a tool you can apply in your daily practice. Here are examples of medications that can affect wound healing. Assessment and care planning for wound healing should include a thorough review of the individual’s current medications to identify those that may affect healing outcomes. Clinicians must then weigh the… Read more…
Each issue, Apple Bites brings you a tool you can apply in your daily practice. Here are examples of medications that can affect wound healing. Assessment and care planning for wound healing should include a thorough review of the individual’s current medications to identify those that may affect healing outcomes. Clinicians must then weigh the… Read more… -
By Nancy Morgan, RN, BSN, MBA, WOC, WCC, DWC, OMS Each issue, Apple Bites brings you a tool you can apply in your daily practice. Here’s an overview of cutaneous candidiasis. Cutaneous candidiasis is an infection of the skin caused by the yeast Candida albicans or other Candida species. Here’s a snapshot of this condition.… Read more…
-
By Nancy Morgan, RN, BSN, MBA, WOC, WCC, DWC, OMS Each issue, Apple Bites brings you a tool you can apply in your daily practice. Here’s an overview of performing a comprehensive skin assessment. In the healthcare setting, a comprehensive skin assessment is a process in which the entire skin of a patient is examined… Read more…
-
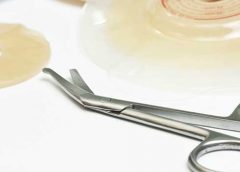
Moldable ostomy barrier rings and strips
By Nancy Morgan, RN, BSN, MBA, WOC, WCC, DWC, OMS Each issue, Apple Bites brings you a tool you can apply in your daily practice. Here’s a brief overview on moldable, bendable, and stretchable adhesive rings and strips used to improve the seal around a stoma. Benefits Adhesive rings and strips can be an alternative… Read more…
-
By Nancy Morgan, RN, BSN, MBA, WOC, WCC, DWC, OMS Each issue, Apple Bites brings you a tool you can apply in your daily practice. Medical gauze, a bleached white cloth or fabric used in bandages, dressings, and surgical sponges, is the most widely used wound care dressing. Commonly known as “4×4s,” gauze is made… Read more…
-
Linear wound measurement basics
By Nancy Morgan, RN, BSN, MBA, WOC, WCC, DWC, OMS Each issue, Apple Bites brings you a tool you can apply in your daily practice. Measurement of wounds is an important component of wound assessment and provides baseline measurements, enables monitoring of healing rates, and helps distinguish among wounds that are static, deteriorating, or improving.… Read more…
-
What you need to know about transparent film dressings
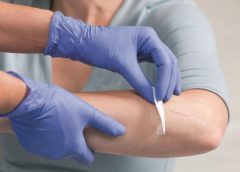 By Nancy Morgan, RN, BSN, MBA, WOC, WCC, DWC, OMS Each issue, Apple Bites brings you a tool you can apply in your daily practice. Transparent film dressings are thin sheets of transparent polyurethane (polymer) coated with an adhesive. These dressings are available in a variety of sizes and shapes. Description Transparent film dressings provide… Read more…
By Nancy Morgan, RN, BSN, MBA, WOC, WCC, DWC, OMS Each issue, Apple Bites brings you a tool you can apply in your daily practice. Transparent film dressings are thin sheets of transparent polyurethane (polymer) coated with an adhesive. These dressings are available in a variety of sizes and shapes. Description Transparent film dressings provide… Read more… -
Understanding the crusting procedure
By Nancy Morgan, RN, BSN, MBA, WOC, WCC, DWC, OMS Each issue, Apple Bites brings you a tool you can apply in your daily practice. The crusting procedure produces a dry surface and absorbs moisture from broken skin through an artificial scab that’s created by using skin barrier powder (stoma powder) and liquid polymer skin… Read more…
-
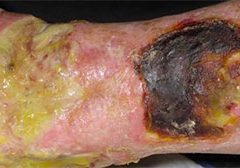 By Nancy Morgan, RN, BSN, MBA, WOC, WCC, DWC, OMS Each issue, Apple Bites brings you a tool you can apply in your daily practice. Exudate (drainage), a liquid produced by the body in response to tissue damage, is present in wounds as they heal. It consists of fluid that has leaked out of blood… Read more…
By Nancy Morgan, RN, BSN, MBA, WOC, WCC, DWC, OMS Each issue, Apple Bites brings you a tool you can apply in your daily practice. Exudate (drainage), a liquid produced by the body in response to tissue damage, is present in wounds as they heal. It consists of fluid that has leaked out of blood… Read more… -
By Nancy Morgan, RN, BSN, MBA, WOC, WCC, DWC, OMS Each issue, Apple Bites brings you a tool you can apply in your daily practice. Description The spiral wrap is a technique used for applying compression bandaging. Procedure Here’s how to apply a spiral wrap to the lower leg. Please note that commercial compression wraps… Read more…
-
What you need to know about hydrogel dressings
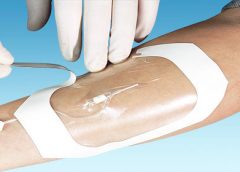 By Nancy Morgan, RN, BSN, MBA, WOC, WCC, DWC, OMS Each issue, Apple Bites brings you a tool you can apply in your daily practice. Description Hydrated polymer (hydrogel) dressings, originally developed in the 1950s, contain 90% water in a gel base, which helps regulate fluid exchange from the wound surface. Hydrogel dressing are usually… Read more…
By Nancy Morgan, RN, BSN, MBA, WOC, WCC, DWC, OMS Each issue, Apple Bites brings you a tool you can apply in your daily practice. Description Hydrated polymer (hydrogel) dressings, originally developed in the 1950s, contain 90% water in a gel base, which helps regulate fluid exchange from the wound surface. Hydrogel dressing are usually… Read more… -
What you need to know about collagen wound dressings
 By Nancy Morgan, RN, BSN, MBA, WOC, WCC, DWC, OMS Description Collagen, the protein that gives the skin its tensile strength, plays a key role in each phase of wound healing. It attracts cells, such as fibroblasts and keratinocytes, to the wound, which encourages debridement, angiogenesis, and reepithelialization. In addition, collagen provides a natural scaffold… Read more…
By Nancy Morgan, RN, BSN, MBA, WOC, WCC, DWC, OMS Description Collagen, the protein that gives the skin its tensile strength, plays a key role in each phase of wound healing. It attracts cells, such as fibroblasts and keratinocytes, to the wound, which encourages debridement, angiogenesis, and reepithelialization. In addition, collagen provides a natural scaffold… Read more… -
What you need to know about xerosis in patients with diabetic feet
By Nancy Morgan, RN, BSN, MBA, WOC, WCC, DWC, OMS Each month, Apple Bites brings you a tool you can apply in your daily practice. Description Xerosis, an abnormal dryness of the skin, is one of the most common skin conditions among patients with type 2 diabetes. While assessing for predictors of foot lesions in… Read more…
-
What you need to know about hydrocolloid dressings
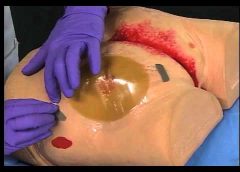 By Nancy Morgan, RN, BSN, MBA, WOC, WCC, DWC, OMS Each month, Apple Bites brings you a tool you can apply in your daily practice. Description A hydrocolloid dressing is a wafer type of dressing that contains gel-forming agents in an adhesive compound laminated onto a flexible, water-resistant outer layer. Some formulations contain an alginate… Read more…
By Nancy Morgan, RN, BSN, MBA, WOC, WCC, DWC, OMS Each month, Apple Bites brings you a tool you can apply in your daily practice. Description A hydrocolloid dressing is a wafer type of dressing that contains gel-forming agents in an adhesive compound laminated onto a flexible, water-resistant outer layer. Some formulations contain an alginate… Read more… -
An Unna boot is a special dressing of inelastic gauze impregnated with zinc, glycerin, or calamine that becomes rigid when it dries. It is used for managing venous leg ulcers and lymphedema in patients who are ambulatory. When the patient walks, the rigid dressing restricts outward movement of the calf muscle, which directs the contraction… Read more…
-
How to do a Semmes Weinstein monofilament exam
By Nancy Morgan, RN, BSN, MBA, WOC, WCC, DWC, OMS Each month, Apple Bites brings you a tool you can apply in your daily practice. Description According to the American Diabetes Association, all patients with diabetes should be screened for loss of protective sensation in their feet (peripheral neuropathy) when they are diagnosed and at… Read more…
-
Sample procedure for nonsterile dressing change
By Nancy Morgan, RN, BSN, MBA, WOC, WCC, DWC, OMS Each month, Apple Bites brings you a tool you can apply in your daily practice. Description • Nonsterile dressings protect open wounds from contamination and absorb drainage. • Clean aseptic technique should be used to change nonsterile dressings. • In the event of multiple wounds,… Read more…
-
By Nancy Morgan, MBA, BSN, RN, WOC, WCC, CWCMS, DWC Each month, Apple Bites brings you a tool you can apply in your daily practice. Description • Semipermeable polyurethane foam dressing • Nonadherent and nonlinting • Hydrophobic or waterproof outer layer • Provides moist wound environment • Permeable to water vapor but blocks entry of… Read more…
-
By Nancy Morgan, MBA, BSN, RN, WOC, WCC, CWCMS, DWC Each month Apple Bites brings you a tool you can apply in your daily practice. Description Dressing with calcium and sodium fibers made from seaweed Spun into rope or flat dressing form Actions Transforms into a moist gel consistency when it comes into contact with… Read more…
