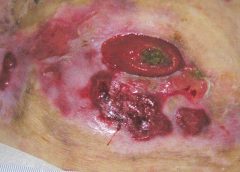
Diabetic foot ulcers stem from multiple factors, including peripheral neuropathy, high plantar pressures, decreased vascularity, and impaired wound healing. Contributing significantly to morbidity, they may cause limb loss and death. (See Foot ulcers and diabetes.)
Initially, hydrocolloid dressings were developed to function as part of the stomal flange. Based on their success in protecting peristomal skin, they were introduced gradually into other areas of wound care. They contain wafers of gel-forming polymers, such as gelatin, pectin, and cellulose agents, within a flexible water-resistant outer layer. The wafers absorb wound exudate, forming a gel and creating a moist healing environment. (more…)
Read More