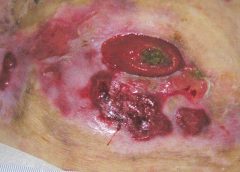
As a wound care specialist, you have learned about many skin conditions, some so unusual and rare that you probably thought you would never observe them. I’ve been a nurse for 38 years, with the last 10 years in wound care, and that’s certainly what I thought. But I was wrong. Let me tell you about my challenging patient with an unusual skin condition.
A perplexing patient (more…)
Read More