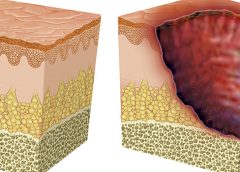
On April 13, 2016, the National Pressure Ulcer Advisory Panel (NPUAP) announced changes in pressure ulcer terminology and staging definitions. Providers can adapt NPUAP’s changes for their clinical practice and documentation, but it’s important to note that, as of press time, the Centers for Medicare & Medicaid Services (CMS) has not adopted the changes. This means that providers can’t use NPUAP’s updates when completing CMS assessment forms, such as the Minimum Data Set (MDS) or Outcome and Assessment Information Set (OASIS). Instead, they must code the CMS assessment forms according to current CMS instructions and definitions. In addition, there is no ICD-10 code for pressure injury. (more…)
Read MoreSearch Results for: docume
Preparing the wound bed: Basic strategies, novel methods
The goal of wound-bed preparation is to create a stable, well-vascularized environment that aids healing of chronic wounds. Without proper preparation, even the most expensive wound-care products and devices are unlikely to produce positive outcomes.
To best prepare the wound bed, you need to understand wound healing physiology and wound care basics, as well as how to evaluate the patient’s overall health and manage wounds that don’t respond to treatment. (See Normal wound healing.) (more…)
Read MoreClinical Notes: biofilm, bariatric surgery, statins and more
Management of biofilm recommendations
The Journal of Wound Care has published “Recommendations for the management of biofilm: a consensus document,” developed through the Italian Nursing Wound Healing Society.
The panel that created the document identified 10 interventions strongly recommended for clinical practice; however, panel members noted that, “there is a paucity of reliable, well-conducted clinical trials which have produced clear evidence related to the effects of biofilm presence.” (more…)
Read More2016 Journal: March – April Vol. 5 No. 2
Clinician Resources: OSHA, Education Program, Civil Workplace
This issue we focus on resources to help clinicians protect themselves from injuries and engage in a healthier lifestyle.
OSHA safety website
A hospital is one of the most hazardous places to work, according to the Occupational Safety and Health Administration (OSHA). The agency provides a wealth of information on how to protect hospital workers as part of its website Worker Safety in Hospitals: Caring for Our Caregivers. PDF resources include:
• A fact sheet that helps dispel myths, barriers, and concerns related to safe patient handling
• Information on making the case for safe patient handling programs (more…)
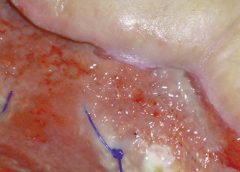
Read MoreCauses, prevention, and treatment of epibole
As full-thickness wounds heal, they begin to fill in from the bottom upward with granulation tissue. At the same time, wound edges contract and pull together, with movement of epithelial tissue toward the center of the wound (contraction). These epithelial cells, arising from either the wound margins or residual dermal epithelial appendages within the wound bed, begin to migrate in leapfrog or train fashion across the wound bed. Horizontal movement stops when cells meet (contact inhibition). The ideal wound edge is attached to and flush with the wound bed, moist and open with the epithelial rim thin, and pale pink to translucent. (more…)
Read MoreA pressure ulcer by any other name
Just when we think we’ve figured out pressure ulcer staging, it changes again. In April 2016, the National Pressure Ulcer Advisory Panel (NPUAP) held a consensus conference on staging definitions and terminology. The purpose: to analyze and discuss the rationale for the panel’s changes. One of the key changes is replacing the term “pressure ulcer” with “pressure injury.” So instead of calling it a pressure ulcer staging system, NPUAP will refer to it as a pressure injury staging system. The panel explained that the new terminology “more accurately describes pressure injuries to both intact and ulcerated skin.” Other changes include: (more…)
Read MoreSubmit an Article
How to submit your article
Submit your manuscript electronically as an MS Word file. Follow these guidelines:
- At the top of the first page of the document, place the article title, your initials (not your name), and the date.
- DO NOT include extra hard returns between lines or paragraphs, extra spaces between words, or any special coding.
- Send a separate cover letter that includes your name; credentials; position; address; home, cell, and work telephone numbers; email address; and your employer’s name, city, and state.
- Email the article and any other attachments to [email protected] and [email protected].
What happens to your manuscript after submittal?
- You will receive an email confirming receipt.
- If your manuscript contains clinical information and we believe it has publication potential, we will send it out for blind peer review (neither you nor the reviewers will know who wrote the article). All manuscripts also receive an internal editorial review. After the review, we’ll let you know whether the manuscript has been accepted, accepted pending revisions, or declined.
- If we accept your manuscript for publication, we’ll ask you to sign an agreement that gives HealthCom Media (publisher of Wound Care Advisor) the rights to your article so that it can be published. Each author must sign a separate agreement.
- Your article will go through our in-house editorial process, where professional editors ensure consistency with our editorial style. You will have a chance to review the edited version before it’s published.
- We will email you if we decide not to publish your manuscript.
Thank you for considering publishing in Wound Care Advisor, the official journal of the National Alliance of Wound Care and Ostomy, the official. If you have any questions, please email: Cynthia Saver, RN, MS, at [email protected] or [email protected].
Read MoreExercise your right to be fit!
Nearly all clinicians know exercise is good for our physical and mental health. But incorporating it into our busy lives can be a challenge. The only types of exercise some clinicians have time for are working long shifts, juggling life’s demands, balancing the books, jumping on the bandwagon, climbing the ladder of success, and skipping meals.
Clinicians are in a unique position to help patients change their behavior to improve their health. Ironically, the first behavior clinicians need to change is to work toward improving our own exercise habits. (more…)
Read MoreNutritional considerations in patients with pressure ulcers
Optimizing nutritional status is a key strategy both in preventing and managing pressure ulcers. In patients across all care settings, compromised nutrition— as from poor intake, undesired weight loss, and malnutrition—increases the risk of pressure ulcers. It contributes to altered immune function, impaired collagen synthesis, and decreased tensile strength. In many cases, malnutrition also contributes to wound chronicity and increases the risk for delayed and impaired wound healing. In patients with chronic wounds, such as pressure ulcers, a chronic inflammatory state can induce catabolic metabolism, malnutrition, and dehydration. (more…)
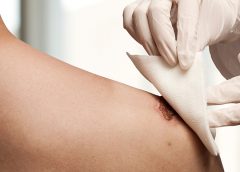
Read MoreNo more skin tears
Imagine watching your skin tear, bleed, and turn purple. Imagine, too, the pain and disfigurement you’d feel.
What if you had to live through this experience repeatedly? That’s what many elderly people go through, suffering with skin tears through no fault of their own. Some go on to develop complications.
A skin tear is a traumatic wound caused by shear, friction, or blunt-force trauma that results in a partial- or full-thickness injury. Skin tears are painful because the precipitating injury commonly involves the dermis, which is rich with nerve endings. (more…)
Read MoreBuzz Report: Latest trends, part 2
Keeping clinicians up-to-date on clinical knowledge is one of the main goals of the Wild on Wounds (WOW) conference held each September in Las Vegas. Every year, I present the opening session, called “The Buzz Report,” which focuses on the latest-breaking wound care news—what’s new, what’s now, and what’s coming up. I discuss new products, practice guidelines, resources, and tools from the last 12 months in skin, wound, and ostomy management.
In the January issue, I discussed some of the updates from my 2015 Buzz Report. Now I’d like to share a few more, along with some of my favorite resources. (more…)
Read More