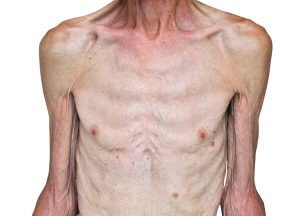
Optimizing nutritional status is a key strategy both in preventing and managing pressure ulcers. In patients across all care settings, compromised nutrition— as from poor intake, undesired weight loss, and malnutrition—increases the risk of pressure ulcers. It contributes to altered immune function, impaired collagen synthesis, and decreased tensile strength. In many cases, malnutrition also contributes to wound chronicity and increases the risk for delayed and impaired wound healing. In patients with chronic wounds, such as pressure ulcers, a chronic inflammatory state can induce catabolic metabolism, malnutrition, and dehydration. (more…)
Read MoreTag: nutrition
Clinician Resources: Nutrition, Treatment Algorithms, Pressure Ulcer Prevention
Check out these resources for your practice.
Be a nutrition champion
One in three patients enters a hospital malnourished. Fight malnutrition by viewing six short videos from the Alliance to Advance Patient Nutrition, including “Rapidly Implement Nutrition Interventions” and “Recognize and Diagnose All Patients at Risk of Malnutrition.” The videos show how to collaborate with the care team to become champions of nutrition and help improve patient outcomes. Watch the videos online or download them for later viewing. (more…)
Read More