By Donna Sardina, RN, MHA, WCC, CWCMS, DWC, OMS
With so much focus on dressing choices, it’s easy to forget the importance of wound cleansing. Cleaning a wound removes loose debris and planktonic (free-floating) bacteria, provides protection to promote an optimal environment for healing, and facilitates wound assessment by optimizing visualization of the wound. You should clean a wound every time you change a dressing, unless it’s contraindicated.
Here’s a review of how to choose and use a wound cleanser so you can see if your practice is up to date.
Choosing a wound cleanser
The ideal wound cleanser is hypoallergenic, nontoxic to viable tissue, readily available, cost effective, and stable. The wound cleanser should also:
• be effective in the presence of organic material, such as blood, slough, or necrotic tissue
• reduce the number of microorganisms that form on the surface of the wound
• have a delivery force less than 15 pounds per square inch.
Common wound cleansers
Below are common types of wound cleansers:
• Normal saline solution. Normal saline solution is the preferred cleansing agent because as an isotonic solution, it doesn’t interfere with the normal healing process. It’s also cost effective and available in many different formats, including unit dose, half liters, liters, and spray bottles.
• Commercial cleansers. Ingredients in commercial cleansers may include surfactants, wetting agents, moisturizers, and/or antimicrobials.
- Surfactants are agents that facilitate removal of wound contaminants. Each surfactant molecule has a hydrophilic (water-loving) head that is attracted to water molecules and a hydrophobic (water-hating) tail that repels water and simultaneously attaches itself to wound contaminants, oils, or grease.
These opposing forces loosen the particles and suspend them in the water.
• Skin cleansers. Skin cleansers are
formulated to remove fecal matter, so they should never be used on open wounds, as they tend to be stronger than a wound cleanser and toxic to wound tissues.
• Lactated Ringer’s solution. Lactated Ringer’s solution provides sodium, potassium, and calcium chloride to the wound, while safely cleaning it and avoiding damage to viable cells. Be careful when the solution is used for continuous irrigation or allowed to dwell inside body cavities; otherwise the solution could be absorbed into the bloodstream, leading to circulatory overload.
• Potable (drinkable) tap water. Potable tap water can be used if there is no other alternative. Check the quality of the water source. Advantages of tap water for wound cleansing are efficiency, cost effectiveness, and accessibility. However, use normal saline solution instead of water for wounds with exposed bone or tendon.
Click here to see examples of wound cleansers.
How to clean a wound
Before you start, make sure the cleansing solution is at room temperature or slighter warmer. It can take up to 40 minutes after cleaning for a wound to regain its original temperature, and up to 3 hours for miotic cell division and leukocytic activity to return to normal.
Once the solution is warm, wash your hands and put on gloves.
View a video on wound cleaning
Manual cleansing technique
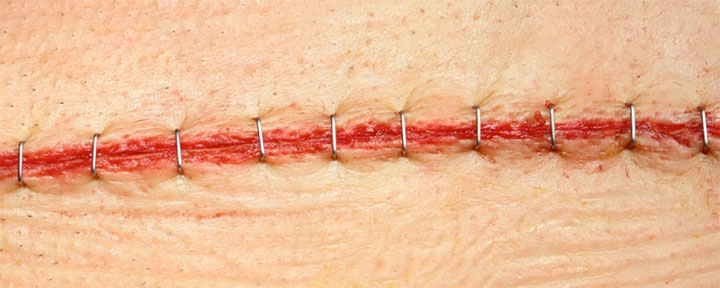
For a linear wound or incision:
1. Pour irrigation solution into the irrigation tray. Moisten clean 4″×4″ gauze pads in the solution; squeeze out excess.
2. Gently wipe the wound from top to bottom in one motion, starting directly over the wound.
3. Discard the used gauze pad.
4. Using a new moistened 4″×4″ gauze pad, repeat cleaning, using a gentle downward stroke parallel to the incision.
5. Repeat steps, working outward from the incision in lines parallel to the incision.
6. Remember to use a new 4″×4″ gauze pad for each downward stroke.
7. If needed, dry the wound, following the same procedure as for cleaning, using dry gauze pads.
For an open wound:
1. Pour the irrigation solution into the irrigation tray. Moisten 4″×4″ gauze pads in the solution; squeeze out excess.
2. Gently clean the wound in a full or half circle, beginning in the center and working toward the outside.
3. Use a new 4″×4″ gauze pad for each circle.
4. Clean at least 1 inch beyond the end of the new dressing or 2 inches beyond the wound margins if you aren’t applying a dressing.
5. If needed, dry the wound, using the same procedure as for cleaning. Gently pat the wound dry, using dry gauze pads.
Spray cleansers
1. Spray cleansers may be applied directly to the wound or sprayed onto clean 4″×4″ gauze pads and then applied to the wound.
2. Check your organization’s policy for required personal protective equipment (PPE). Generally, wound irrigation
that involves squirting, spraying, or pressure release of fluid will require the use of PPE (such as gloves, gown, and mask with eye shield) to prevent exposure to debris and airborne microorganisms.
3. Protect the environment, equipment, and other supplies from contamination from spray aerosolization by covering or removing the supplies.
4. Hold the spray bottle approximately
1 inch from the wound bed. Aim the nozzle at the wound and squeeze the bottle, directing the stream of cleanser along the base and sides of the wound.
5. Blot up excess moisture with a clean gauze pad.
6. Dry the surrounding skin.
Cleaning with a saline bullet
1. Position the patient so that the cleansing solution will flow by gravity from the upper end of the wound to the lower end.
2. Twist off the top.
3. Position the container at any angle required to access the area to be moistened or cleaned.
4. Apply firm pressure to the container to obtain the desired flow rate.
5. Blot up excess moisture with a clean gauze pad.
6. Dry the surrounding skin.
After you have finished cleaning the wound, dispose of the waste in a trash bag; then remove and discard your gloves and any other PPE you used.
Selected references
European Pressure Ulcer Advisory Panel and National Pressure Ulcer Advisory Panel. Treatment of pressure ulcers: Quick reference guide. Washington, DC: National Pressure Ulcer Advisory Panel; 2009.
Hess CT (ed.). Clinical Guide to Wound Care. 7th ed. Philadelphia, PA: Lippincott Williams & Wilkins; 2012.
Kosier B. Fundamentals of Nursing: Concepts, Process, and Practice. 6th ed. Upper Saddle River, NJ: Prentice-Hall, Inc; 2000.
Ovington LG. Hanging wet-to-dry dressings out to dry. Adv Skin Wound Care. 2002;15(2):79-84.
Wound Source. Wound cleansers. http://www.woundsource.com/product-category/wound-cleansers/wound-cleanser-products. Accessed April 1, 2013.
Donna Sardina is Editor-in-Chief of Wound Care Advisor and cofounder of the Wound Care Education Institute in Plainfield, Illinois.








I am a new nurse working in an urgent care center. This feature article would be of great help in my practice. Thanks!
there is a controversey at work if you need to change gloves and wash hands prior to applying clean treatment/dressing
Kelly,
Here is a quick description of glove changing according to infection control guidelines:
1-Wash hands, apply gloves
2- Remove soiled dressing
3- Remove gloves, wash hands, apply new gloves.
4- Clean wound with prescribed cleanser
Pat the tissue surrounding the wound dry
5- Remove gloves, wash hands, apply new gloves.
6-Apply wound dressing
7-Discard gloves and all used supplies in trash bag
8- Wash hands
Also, Here is a link to a detailed step by step procedure of non-sterile dressing change. http://woundcareadvisor.com/apple-bites-vol1-no4/
Thank you for your post regarding washing hands and donning new gloves. It just seems wrong to be advised not to change gloves after cleansing a wound thereby potentially infecting a wound.
You are correct. Gloves should be removed and hands washed after cleaning a wound.
4- Clean wound with prescribed cleanser. Pat the tissue surrounding the wound dry.
5- Remove gloves, wash hands, apply new gloves
Can I change the ratio of the saline solution? Will it make any difference?
Thank you for the technique
Please I have observed a wound dressing in which savlon and Hydrogen Peroxide used. Why should they be used?
What cleanser do I use on a beefy red wound? Thanks
Normal saline, a commercial wound cleanser, or even clean tap water can be used.
I’m currently undergoing treatment after a bike accident. The nurses clean the wound very hard and have use a scalpel once to scrap some wounds after a few days if healing!
I feel that the wounds are taking to long to heal because of the hard cleaning! They told me they want to scrap my knee ( after 10 days already ) today which will be very painful. I feel like the hospital is prolonging the treatment which I’m paying for PLEASE ADVISE thank you!
Without seeing your wound, I cannot tell you if your treatment is correct. However, cleaning a wound is important to make sure it heals correctly. Cleaning can also involve a method called debridement. Debridement is the removal of dead, dry or infected tissue from the wound bed. Scrubbing and scalpel use are both considered forms of debridement. There are other methods of debridment that can be used, some of which take longer for healing to occur, but are less painful. Here is a link to an article that discusses wound debridement http://woundcareadvisor.com/debridement-options-beams-made-easy_vol2-no/
Hope this helps
l’m an infection control nurse and just back from post basic in infection control l was taught not to use Normal saline solution for wound cleaning as it will enhance the growth of microorganism. Could you please advice.
Rafizah, I am not familiar with any studies or practices that state normal saline will enhance growth of microorganisms in a wound. However, commercial normal saline generally does not contain a preservative to prevent bacteria from growing in the container. Therefore, one opened, saline bottles should be discarded within 24 hours of opening.
My mom is bedridden and is paralyzed. We turn her every 2-3 hours so that she doesn’t get sores. A few days ago, I noticed the side of the right buttock looking irritated so I cleaned it and put duoderm and covered it with tegaderm. However it turned into a blister. When it popped I continued to clean and put dressing on it. A couple of days later, the wound continued to saturate the bandage with a liquid that had a bad smell. Last night I pressed on the wound to try to see if there is more liquid underneath, and since it had a bad smell I worried about infection. Once I pressed on it, more liquid did come out, and the skin gave way, and I could see a deep wound underneath that I couldn’t tell was there when the skin was still over it. What do I do? Should I take her to the emergency room, or is this something I can take care of at home? I will talk to my cousin who is a physician’s assistant to get advice, but help from someone who specializes in wound care would be so very much appreciated. I hesitate to take my mom to the emergency only because last time it took them hours before they took a look at her and I would hate to have her sit in her wheelchair uncomfortable. Thanks for any advice you can give!
Yes, your moms wound does need to be seen by either a physician, nurse practitioner, or wound specialist. Infection in wounds can spread into the bloodstream easily causing serious problems and even death if not treated promptly.
I am doing research on wound irrigation. We are a rural hospital and rely upon irrigating wounds with a 35 ml syringe and 18g catherer, using normal saline. Or we have tips that can be applied directly to saline bottles. Can you direct me to articles for EBP guidelines and what are your thoughts on irrigating tunnels?
Can you explain the implications of wound healing when saline from the fridge is used? Is it okay to put NS in fridge? Thank you
Donna,
Are normal saline bullets really adequate for therapeutic wound cleansing? I am concerned that the size of saline bullets are insufficient to properly cleanse a wound/ulcer and question if they have a PSI appropriate for wound cleansing. Please elaborate…Thank you Donna
Am wondering if in after cleaning an open wound, it is better to pack with equal a n b or iodine
Thanks a lot for refreshing my memory
skin care las vegas
We use a dermal wound cleanser in a spray bottle in office. I cannot find a set time to discard unused portion of wound cleanser (ie saline is 24 hrs) after opening. Is there a time limit or is it just manufacturer’s date?
I had surgery in jan 2016, my wound is still opened, bleeding and constantly infected. Should the district nurse use tap water to clean the open wound before applying a iodine solution