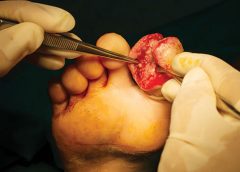
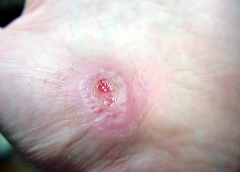
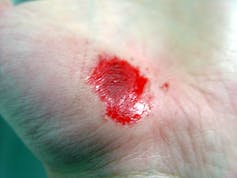
Nurses and therapists often wonder if their license permits them to perform sharp wound debridement. Scope of practice varies significantly from state to state, so it’s imperative to check your state for specific guidance, but we can address some of the challenges clinicians face in deciding whether they can perform this valuable service for patients.
Search Results for: Debr
Clinical Notes: Debridement, Optimal Wound Healing, Diabetes, Sacral Wounds
Frequent debridement improves wound healing
A study in JAMA Dermatology reports that frequent debridements speed wound healing.
“The more frequent the debridement, the better the healing outcome,” concludes “Frequency of debridements and time to heal: A retrospective cohort study of 312 744 wounds.” The median number of debridements was two.
Most of the wounds in the 154,644 patients were diabetic foot ulcers, venous leg ulcers, and pressure ulcers. The study authors note that debridement is a “key process” in wound bed preparation and starting the healing process.
The findings are congruent with previous studies and are based on an analysis of the largest wound data set to date. (more…)
Read MoreDebridement options: BEAMS made easy
By Cindy Broadus, RN, BSHA, LNHA, CHCRM, CLNC, CLNI, WCC, DWC, OMS
At one time or another, all wound care professionals encounter a chronic wound, defined as a wound that fails to heal in an orderly and timely manner. Globally, about 67 million people (1% to 5% of the world’s population) suffer chronic wounds. In the United States, chronic wounds affect 6.5 million people and cost more than $25 billion annually to treat. (more…)
Read MoreWhy do older people heal more slowly?
By Matthew Steinhauser, University of Pittsburgh
I recently visited an 83-year-old patient in the hospital after EMTs rushed her to the ER with an infected leg wound. Her ordeal started inconspicuously when she bumped into the sharp edge of a table and developed a small cut. The patient’s wound didn’t close, but she ignored it until she woke up in pain one morning two weeks after first injuring her leg. Her daughter called 911 after noticing angry, red skin discoloration and pus – both signs of an infection. Our medical team treated her with IV antibiotics and cleared up the infection, but the wound did not fully close until at least a month later, well after she was discharged from the hospital.
How different the story is when children get a cut. They may scream initially, but within days, the scab falls off, revealing new skin. Why was healing so delayed in my 83-year-old patient compared to a healthy child?
The answer is age. Decades of life slow down healing for most tissues, and wounds in skin can offer a window into why this slowdown occurs.
Three stages of wound healing
I am physician who studies how aging predisposes patients to diseases like diabetes and whether behavioral changes such as intermittent fasting may slow down aging. In order to understand why the skin wound in my older patient healed so slowly, it is important to first understand how wounds heal under the ideal conditions of youth.
The wound healing process is classically categorized into three stages.
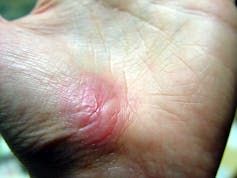
Right after a wound occurs, the inflammatory response begins.
Jpbarrass via Wikimedia Commons
The first stage is inflammation, essentially the body’s attempt to clean the wound. During the inflammatory phase, immune cells called phagocytes move into the wound, kill any contaminating bacteria, and ingest and dispose of dead cells and debris.
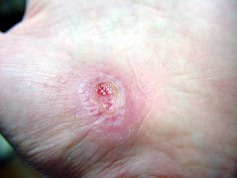
Jpbarrass via Wikimedia Commons
Inflammation sets the stage for the regenerative phase, where several processes work in concert to regrow damaged skin. Replacement skin cells are born when cells at the edge of the wound divide, while fibroblast cells lay down a supportive scaffolding called the extracellular matrix. This holds the new cells together. Any damaged supporting structures of the skin, such as the blood vessels that supply critical oxygen and nutrients, also need to regrow. The second stage effectively closes the wound and restores a protective barrier against bacteria.
Jpbarrass via Wikimedia Commons
The regenerative phase is a relatively quick, but tenuous fix – new skin is fragile. The final remodeling phase plays out over a couple of years as the new skin is progressively strengthened by several parallel processes. The extracellular matrix, which was initially laid down in a haphazard fashion, is broken down and replaced in a more durable way. Any residual cells from prior phases that are no longer needed – such as immune cells or fibroblasts – become inactive or die. In addition to strengthening the new skin, these collective actions also account for the tendency of scars to visibly fade with time.
Products
Diseases disrupt the healing process
One major way aging can derail the orderly and efficient progression through the stages of healing is through the health problems that stem from diseases of old age.
Diabetes is one example of a disease that is strongly associated with older age. One of the many ways that diabetes negatively affects healing is by causing blood vessels to narrow. As a consequence of inadequate circulation, crucial nutrients and oxygen do not reach the wound in sufficient quantities to fuel the second regenerative phase.
Diabetes is just one of many age-related diseases that disrupts normal processes in the body such as wound healing.
Cells age too
Aside from the negative impacts of age-associated diseases, cells themselves age. In an extreme sign of aging called cellular senescence, cells permanently lose the ability to divide. Senescent cells accumulate in skin and many other organs as people age and cause a host of problems.
When cells divide more slowly – or when they stop dividing altogether due to senescence – skin becomes thinner. The replacement of fat cells, which form a cushioning layer under the skin, also declines with age. The skin of older patients is therefore more prone to injury in the first place.
Once an older person’s skin is injured, the skin has a harder time healing properly as well. Aging and senescent immune cells cannot defend against bacteria, and the risk of serious skin infection rises. Then in the regenerative stage, slow rates of cell division translate into slow skin regrowth. My patient exhibited all of these negative effects of age – her thin, almost translucent skin ruptured from a minor bump, became infected and took nearly two months to fully regrow.
But senescent cells are more than just dysfunctional bystanders. For reasons that are not yet fully understood, senescent cells release toxic byproducts that damage surrounding tissue and drive inflammation – even when there’s no bacterial threat present. Some of these byproducts can even accelerate senescence in neighboring cells. This suggests that intrinsic aging of cells is in essence contagious and senescent cells actively fuel an uncontrolled cycle of inflammation and tissue damage that further impedes successful regeneration and healing.
A whole body problem
As the most outwardly visible tissue of the body, the skin provides a window into why people heal more slowly with age, but all tissues can be injured and are susceptible to the effects of aging. Injuries may be small, repetitive and build up over time – like the effect of smoking on the lungs. Or they may be discrete and dramatic – such as the death of heart cells with a heart attack. Different tissues may heal in different ways. Yet all tissues share a sensitivity to the repercussions of an aging immune system and a decline in the ability to regrow dead or damaged cells.
Understanding why healing slows down with age is important, but my patient asked a very practical question that physicians often face in one form or another: “Doctor, what can you do for me?”
Unfortunately, current treatment of wounds is fairly old-fashioned and often ineffective. Some of the options available include wound dressing changes, antibiotics when the wound is infected or treatment in a high oxygen chamber when circulation is bad due to diabetes.
There is hope, though, that medicine can do better and that progress in understanding the aging process will lead to new therapies. Neutralizing senescent cells in mice, for example, improves a variety of age-associated diseases. While it is way too early to say that researchers have discovered the fountain of youth, I am optimistic for a future when physicians will bend the aging curve and make skin and other organs heal faster and better.
Matthew Steinhauser, Associate Professor of Medicine, University of Pittsburgh
This article is republished from The Conversation under a Creative Commons license. Read the original article.
Antibiotic use in pressure injury infections
Antibiotic overuse contributes to the problems of antibiotic resistance and healthcare acquired infections, such as Clostridium difficile. Antibiotic stewardship programs improve patient outcomes, reduce antimicrobial resistance, and save money. These programs are designed to ensure patients receive the right antibiotic, at the right dose, at the right time, and for the right duration. (more…)
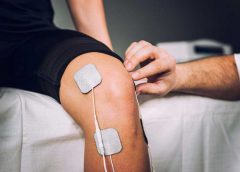
Read MoreHow to benefit from electrical stimulation for the treatment of chronic wounds
One of the most amazing things about the human body is its ability to repair itself. Lacerations, punctures, abrasions all heal with little or no care. Chronic wounds, those that persist day after day, are a small subset of wounds but they compose a troublesome minority. They include, but are not limited to, diabetic foot ulcers (DFU), venous leg ulcers (VLU), and pressure ulcers (colloquially known as bedsores). These represent the body’s failure to fix itself. (more…)
Read MoreNecrotizing Fasciitis: Pearls & Pitfalls
A 39-year-old woman presents to the ED with leg pain and fever. She initially noted redness and pain above her knee 2 weeks ago and was evaluated at an outside hospital. She completed a 10-day course of oral antibiotics for cellulitis. Over the last two days, she has had progressive leg swelling of her entire right thigh. The pain is now so severe that she is having difficulty walking. Her past medical history is negative for diabetes mellitus, chronic liver disease, or alcohol and IV drug use.
On exam, she is febrile to 102.7 F, heart rate is 96 bpm, and blood pressure is 112/65. She has a 12 cm area of faint erythema on her right thigh and tenderness to palpation of her entire right leg with diffuse edema. There is no ecchymosis or bullae formation. (more…)
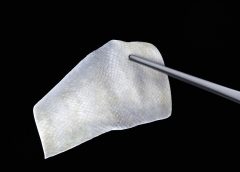
Read MoreFish Skin for Human Wounds: Iceland’s Pioneering Treatment
The FDA-approved skin substitute reduces inflammation and transforms chronic wounds into acute injuries.
Six hours north of Reykjavik, along a narrow road tracing windswept fjords, is the Icelandic town of Isafjordur, home of 3,000 people and the midnight sun. On a blustery May afternoon, snow still fills the couloirs that loom over the docks, where the Pall Palsson, a 583-ton trawler, has just returned from a three-day trip. Below the rust-spotted deck, neat boxes are packed with freshly caught fish and ice. “If you take all the skins from that trawler,” says Fertram Sigurjonsson, the chairman and chief executive officer of Kerecis Ltd., gesturing over the catch, “we would be able to treat one in five wounds in the world.” (more…)
Read MoreAtrium Medical Center division earns award for clinical excellence
MIDDLETOWNThe Wound Care Center and Hyperbaric Services at Atrium Medical Center recently was recognized with a national award for clinical excellence.
The Center of Distinction Award was presented by Healogics, the nation’s leading and largest wound care management company. The center was also honored with the Healogics President’s Circle Award.
The awards recognize outstanding clinical outcomes for 12 consecutive months, including patient satisfaction higher than 92 percent, and a wound healing rate of at least 91 percent in less than 31 median days. (more…)
Read MoreLaughlin Center Named Wound Care Center Of The Year
Laughlin Center for Wound Care and Hyperbarics has been honored as the Wound Care Center of the Year as well as recognized with a national award for continued excellence in wound healing by Healogics Inc., a wound care management company.
Leaders, physicians and clinicians from Laughlin Center for Wound Care and Hyperbarics recently gathered to celebrate the center’s receipt of the Robert A. Warriner III Center of Excellence award, according to a news release.
Control your claims: Pressure ulcer/wound care management
One of many dreaded tags from a Centers for Medicare & Medicaid Survey is F-Tag 314 — Pressure ulcers.
CMS writes, “Each resident must receive and the facility must provide the necessary care and services to attain or maintain the highest practicable physical, mental, and psychosocial well-being, in accordance with the comprehensive assessment and plan of care.” (more…)
Read MoreCovenant Health Wound Care Experts Earn National, Regional Recognition
LUBBOCK, TX (NEWS RELEASE) – The Covenant Center for Wound Care & Hyperbaric Medicine has been honored as a Wound Care Center® of the Year by Healogics, Inc., the nation’s leading and largest wound care management company. The center also was awarded Center of Distinction and the President’s Circle Award.
The center has achieved patient satisfaction rates higher than 92 percent, a healing rate of at least 91 percent in less than 31 median days and healed almost 90 percent of its patients in less than 14 weeks. Out of the 630 Centers eligible in 2016, only seven centers across the country received this prestigious award. Covenant’s center was awarded as Center of the Year for the southwest region, which includes Texas, Oklahoma, Louisiana and New Mexico. (more…)
Read More