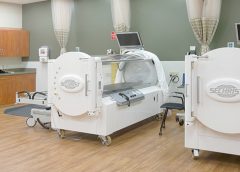
Why would a patient with a wound spend almost 2 hours a day, 5 days a week, in a locked chamber receiving 100% oxygen? The answer is that medical grade hyperbaric oxygen therapy (HBOT) can be a valuable adjunct therapy for selected types of wounds.
In this article, I’ll focus on hospitals and clinics that follow guidelines from the Undersea & Hyperbaric Medical Society as I give you a brief overview of how HBOT works and its use in wound care. (more…)
Tag: hyperbaric oxygen therapy
Medicare reimbursement for hyperbaric oxygen therapy
By Carrie Carls, BSN, RN, CWOCN, CHRN, and Sherry Clayton, RHIA
In an atmosphere of changing reimbursement, it’s important to understand indications and utilization guidelines for healthcare services. Otherwise, facilities won’t receive appropriate reimbursement for provided services. This article focuses on Medicare reimbursement for hyperbaric oxygen therapy (HBOT). (See What is hyperbaric oxygen therapy?)
Indications and documentation requirements
Read MoreHyperbaric oxygen therapy for treatment of diabetic foot ulcers
By Carrie Carls, BSN, RN, CWOCN, CHRN; Michael Molyneaux, MD; and William Ryan, CHT
Every year, 1.9% of patients with diabetes develop foot ulcers. Of those, 15% to 20% undergo an amputation within 5 years of ulcer onset. During their lifetimes, an estimated 25% of diabetic patients develop a foot ulcer. This article discusses use of hyperbaric oxygen therapy (HBOT) in treating diabetic foot ulcers, presenting several case studies.
HBOT involves intermittent administration of 100% oxygen inhaled at a pressure greater than sea level. It may be given in a:
• multi-place chamber (used to treat multiple patients at the same time), compressed to depth by air as the patient breathes 100% oxygen through a face mask or hood (more…)