By Jackie Doubleman, BSN, RN, CWOCN
Most patients are distressed to learn they need ostomy surgery to divert stool, urine, or both. Adapting to ostomy surgery can be difficult at best, even with today’s advanced technology and the wide assortment of ostomy supplies available. While recovering from the surgery itself, patients must learn how to contain or control feces or urine and how to minimize odor—without feeling like a social outcast.
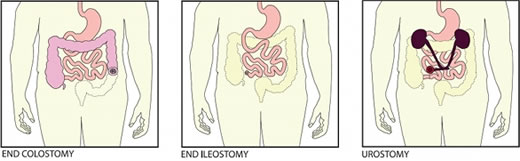
This article reviews three types of ostomy surgery—colostomy, ileostomy, and urostomy. Subsequent articles will discuss ostomy management and treatment of stomal and peristomal skin complications.
Colostomy
A colostomy may be done on any part of the colon. It may be permanent or temporary.
- A permanent colostomy is done when the rectum must be removed or other health problems prevent colostomy closure.
- A temporary colostomy is created to divert stool away from the diseased portion of the colon or large intestine, giving the affected part of the bowel time to rest and heal. Depending on the healing process, the patient may need the colostomy for a few weeks to a few months. Once the affected area is healed, the colostomy can be closed or reversed. Occasionally, a patient may opt to keep the colostomy due to fear of needing another surgery. (See Colostomy indications by clicking the PDF icon above.)
Types of colostomies include ascending, transverse, and descending and sigmoid colostomy. Refer to the image below, which shows the normal intestines, as you read the descriptions.
Ascending colostomy
In this type of colostomy, the surgeon diverts the bowel to an opening in the abdominal wall, rolls the bowel back onto itself, and stitches it to the abdominal wall. The stoma is on the right side of the abdomen, on the ascending portion of the colon. Because stool is diverted from most of the colon, the output is liquid and full of digestive enzymes. The skin must be protected from the effluent and the patient must wear a drainable pouch at all times.
Transverse colostomy
Two types of transverse colostomies are done—loop transverse colostomy and double-barrel transverse colostomy. Usually, they serve as temporary fecal diversions.
- In transverse loop colostomy, the surgeon creates one stoma with a proximal and distal opening. The proximal opening expels stool while the distal opening eliminates mucus. This procedure allows the distal portion of the colon to rest and heal; once it heals, the colostomy may be closed. Normally, a small amount of stool and mucus is expelled from the anus.
- The double-barrel transverse colostomy rarely is done today. The surgeon completely divides the bowel, leaving two stomas on the abdominal wall—a proximal stoma that expels stool and a distal stoma that passes mucus. The distal stoma also may be called a mucous fistula, with the mucus expelled through the rectum. If the two stomas are separated on the abdominal wall, the patient wears a pouch over the proximal stoma to collect feces and wears a piece of plain gauze, a Vaseline gauze pad, or a small pouch called a stoma cap over the mucous fistula stoma. If the stomas are near each other, a single pouch may cover both.
Descending colostomy and sigmoid colostomy
In these procedures, the stoma is on the left lower abdominal wall. The descending colostomy stoma is located just a few inches higher than the stoma for a sigmoid colostomy. A sigmoid colostomy, the most common colostomy type, may be permanent or temporary.
Abdominal perineal resection of the rectum is done in patients with distal rectal cancer. Today, with advanced technology in surgical instrumentation, surgeons may be able to accomplish a lower anastomosis in the rectum and thus prevent a permanent colostomy. If the rectum has been removed, the sigmoid colostomy is permanent. The patient may have the option to regain control over elimination through colostomy irrigation on a regular basis to stimulate peristalsis and evacuate the colon at a designated time. To be eligible for colostomy irrigation, the patient must have had only one or two bowel movements daily before becoming ill and requiring surgery, and must be functionally able to perform irrigation. Because descending and sigmoid colostomies are done in the left lower quadrant, more of the colon is functional; therefore, fecal output usually has a soft to firm consistency.
Ileostomy
With an ileostomy, bowel diversion surgery is restricted to the small intestine on the lower right abdominal wall and affects only the ileum. An ileostomy may be permanent or temporary, depending on whether the rectum was removed. Indications for ileostomy surgery include ulcerative colitis, Crohn’s disease, familial polyposis, and cancer.
Because the colon is removed or bypassed, stool is liquid to semisoft and appears green. The patient must learn to avoid dehydration and will need to wear an external ostomy bag 24 hours daily for fecal collection. Types of ileostomies include the ileoanal reservoir and the Barnett continent intestinal reservoir (BCIR).
Ileoanal reservoir
Also known as the J-pouch or a continent diversion, the ileoanal reservoir is an internal pouch formed from the small intestine. It’s a widely accepted treatment option for patients with ulcerative colitis and familial polyposis because it eliminates the disease and doesn’t require a permanent ileostomy.
This complex procedure most often is done in two stages. In the first procedure, the surgeon removes the colon but leaves the anus intact and disease free; a temporary ileostomy is created to divert stool from the new J-pouch to promote healing. Usually within 4 to 8 weeks, the second surgery is done to take down the ileostomy. Afterward, the patient has six to ten bowel movements per anus daily. After a few months of adjustment, the patient may have only three to six bowel movements daily.
For critically ill patients who need emergency surgery, the surgeon may opt to do a three-stage procedure. The first surgery is a total colectomy with rectal sparing and a temporary loop ileostomy. In the second, the surgeon constructs the J-pouch. The third is ileostomy takedown or reversal.
BCIR
An intra-abdominal ileostomy, the BCIR is used for patients who’ve had problems with conventional ileostomy and difficulty wearing an external ostomy bag, as well as those who’ve failed with the Kock pouch, ileoanal anastomosis, or J-pouch. The BCIR was modified from the Kock pouch (a continent ileostomy) by Dr. William Barnett when he constructed the “living collar,” which is made from the small intestine and helps prevent leakage around the stoma. The Kock pouch is an internal pouch that stores liquid stool (600 to 1,000 ml) and is emptied with a catheter at the patient’s convenience two to four times daily. The stoma empties directly into the toilet. Most patients cover the stoma site with a small pad or bandage to absorb the mucus that accumulates at the opening. As with any diversion, mucus formation at the stoma site is natural because the intestine normally produces mucus.
Urostomy
Also called a urinary diversion, a urostomy is indicated for cancer, bladder extrophy, neurogenic bladder, interstitial cystitis, and ureter blockage caused by a kidney stone or tumor. A urostomy can be one of several types. This article describes the ileal conduit, neobladder, Indiana pouch, Miami pouch, and nephrostomy.
Ileal conduit
Because of its low complication rate and high patient satisfaction, an ileal conduit is the most common urinary diversion technique after a radical cystectomy for invasive bladder cancer. The conduit is created from the terminal ileum of the small intestine. The surgeon resects the ureters from the bladder and performs ureteroenteric anastomosis. After closing one end of the conduit, the surgeon brings the other end through a premarked site in the right lower quadrant of the abdominal wall, creating a stoma.
The goal of an ileal conduit is to expel urine directly from the conduit via the stoma into an external pouch. Patients wear a urinary pouch 24 hours daily and must empty it several times a day. Because they don’t feel the urge to urinate, they must learn to empty the pouch when they feel it getting heavy with urine. They empty it directly into the toilet through the spout on the end. Usually, the pouch is changed two or three times per week. Patients with good wear time and no peristomal skin irritation may need to change it only once a week but must drink at least eight glasses of liquid daily to prevent ascending urinary tract infection.
Neobladder
This continent urinary diversion is done in patients whose bladder has been removed due to cancer. It closely mimics the urinary bladder’s storage function. The surgeon makes part of the small intestine into an internal reservoir and sews it to the urethra. The ureters are attached to drain into the reservoir, providing a downward urine flow to prevent urine back-up and thus help prevent kidney infection. Urine passes from the kidney down the ureters to the reservoir and through the urethra, as in normal urine passage.
Candidates for neobladder surgery must have a low risk of urethral cancer recurrence and be highly motivated to follow a strict care regimen for the first few months. After surgery, they lack the normal urge to urinate, so for the first few months they must void “by the clock.” Initially, they experience nocturnal incontinence, but urinary leakage during the day is unlikely. The neobladder continues to enlarge and function better over the first few years.
The main advantage of this surgery is that with time and patience, the patient can use the bathroom to urinate the same way as before surgery. Neobladders usually are done on men because the female internal anatomy makes neobladder creation much more difficult.
Indiana pouch
The Indiana pouch is used for urinary diversion after bladder cancer, pelvic exenteration, bladder extrophy, or neurogenic bladder. Patients with this continent reservoir must catheterize it to empty stored urine.
The Indiana pouch is created from approximately 2′ of the ascending colon.
The surgeon brings a small portion of the ileum and the end segment through the abdominal wall to create a stoma. The ileocecal valve is included in the reservoir and functions as a one-way valve to help prevent urinary leakage from the stoma.
The patient leaves the hospital using leg bags connected to one tube through the stoma and into the reservoir, and connected to another tube through a temporary opening into the abdominal wall and reservoir. After sufficient healing, the stomal tube is removed and the patient is taught to catheterize the stoma or pouch every 2 hours. After 1 month, if X-rays don’t show urine leakage from the pouch, the last drainage tube is removed. Then the patient catheterizes the pouch every 3 hours around the clock. As the pouch continues to expand, emptying time may increase to 4 or 6 hours, with pouch capacity up to 1,200 ml.
Patients need to irrigate the pouch daily with 60 ml sterile water to remove mucus, salts, and bacteria. After about 6 months, they usually can sleep through the night without emptying the pouch if they limit liquid intake in the evening.
Miami pouch
Another type of continent urostomy, the Miami pouch is created by a gynecologic oncologist at the time of an anterior or total pelvic exenteration. It’s constructed using the distal ileum and ascending colon. Continence is developed with tapering of the ileum, intussusception of the ileal cecal valve, and detubularizing of the colonic segment. With this pouch, pressure is lower than urethral pressure entering it and lower than that of the
efferent bowel leaving it, reducing risk of urinary reflux.
The Miami pouch has proven to be reliable in terms of continence and protecting the upper urinary tract. The most common complications are urethral stricture, difficulty with catheterization, and pyelonephritis. Quality of life improves after a Miami pouch or Indiana pouch continent urostomy because these procedures avoid an external pouch, even though they require intermittent self-catheterization.
Nephrostomy
A nephrostomy is an artificial opening created between the skin and kidney by a surgeon or interventional radiologist. Using ultrasound guidance or computed-tomography fluoroscopy, the practitioner places a catheter in the renal pelvis.
This procedure is done to prevent kidney damage related to urinary blockage. The nephrostomy tube allows the kidney to function properly and protects it from further damage and possible infection; once the condition necessitating the nephrostomy has been treated or corrected, the tube can be removed. If it must remain in place for an extended time, it must be exchanged periodically.
The patient wears an external urostomy pouch over the tube. Depending on individual circumstances, patients may have bilateral nephrostomy tubes or a left or right nephrostomy tube. If only one kidney is blocked, one neophrostomy tube will be placed; the patient voids normally and has to keep the neophrostomy pouch emptied. The nephrostomy tube may need to be irrigated regularly in a sterile procedure, as ordered by the surgeon.
Help patients resume active lives
When confronted with the need for a fecal or urinary diversion, all patients and their families have concerns and questions, and many feel frightened and isolated. Refer them to a local ostomy support group or the United Ostomy Associations of America to help them get through this transition period.
Every patient has the right to be clean, dry, and odor free. To achieve this goal and resume a normal lifestyle, patients must learn about ostomy management. Quality of life after a fecal or urinary diversion can improve if patients understand about the specific surgery required and learn how to perform self-care. Patients with any type of continent fecal or urinary diversion should wear a medical alert medallion in case they are unconscious in an emergency situation. Once patients know how to care for themselves, they can resume full, active lives. Time, patience, and a good sense of humor can help them live life and enjoy it despite the ostomy.
Selected references
Beitz JM. Continent diversions: the new gold standard of ileoanal reservoir and neobladder. Ostomy Wound Manage. 2004;50(9):26-35.
Beitz JM, Gerlach M, Ginsburg P, Ho M, McCann E, et al. Ostomy Wound Manage. 2010;56(10):22-38.
Colwell JC, Goldberg MT, Carmel JE. Fecal and Urinary Diversions: Management Principles. Philadelphia, PA: Elsevier; 2004.
Costa JA, Kreder K. Urinary diversions and neobladders. Medscape Reference: Drugs, Diseases and Procedures. Updated May 16, 2012. http://emedicine.medscape.com/article/451882-overview. Accessed February 28, 2013.
Geng V, Eelen P, Fillingham S, Holroyd S, Kiesbye B, et al. Good Practice in Health Care: Continent Urinary Diversion. Arnhem, The Netherlands: European Association of Urology Nurses; 2009.
Gordon PH. Intestinal stomas. In: Gordon PH, Nvatvongs S, eds. Principles and Practice of Surgery for the Colon, Rectum and Anus. 3rd ed. CRC Press; 2007.
Gutman N. Colostomy Guide. United Ostomy Associations of America; 2011.
Herlufsen P, Olsen AG, Carlsen B, Nybaek H, Karlsmark T, et al. Study of peristomal skin disorders in patients with permanent stomas. Br J Nurs. 2006; 15(16):854-62.
Nie A, Douglas E. Pediatric Ostomy Care: Best Practice for Clinicians. WOCN Society Annual Conference: New Orleans, Louisiana; 2011.
D’Orazio M, Ozorio C. On the lack of universal ostomy follow-up. J Wound Ostomy Continence Nurs. 2008;35(3):313-15.
United Ostomy Associations of America. What is an ostomy? www.ostomy.org/ostomy_info/whatis.shtml. Accessed February 28, 2013.
Jackie Doubleman is a certified wound and ostomy care nurse at St. Vincent’s Hospital in Birmingham, Alabama.







I have been a belly sleeper for a long time. Once I get into a deep sleep I tend to roll over on my belly and I either break the addheasive seal or something else that causes a leak from the stoma and a wet bed
you can try a belly band belt that goes around your tummy and hold the bag in place. It’s made of soft cotton so it doesn’t restrict. you can find them at a ostomy supply store. hope this helps
Is there a way to prevent uti’s. I have been in the hospital several times for them since my surgery last December.
Is there anyway to reverse the indiana pouch surgery and wear bag on the outside instead. My sis has been in and out of the hospital 8 times in the last 2 months due to this surgery. She developed septis twice, constantly vomiting and nauseated and doctors cant find whats wrong other than septis.
My sister has been on this colostomy thing for two months however there is still a bit of drainage coming from the stitched area at the belly and also from the stoma, please is it normal.