By Lydia Meyers, BSN, RN, CWCN
Necrotizing fasciitis (NF) results from an infection that attacks the fascia and subcutaneous tissues. The primary bacterial etiology is group A streptococcus, a facultative anaerobic bacterium. However, other bacteria may contribute. Sometimes called the “flesh-eating” disease because of the potentially devastating effect on the afflicted patient, NF can be monomicrobial or polymicrobial.
The four typical settings for NF are:
- surgical bowel or abdominal trauma surgery
- pressure ulcer and perianal abscess
- injection sites (especially in drug users)
- Bartholin abscess or minor vulvovaginal infection.
Because of the rapid course and ravaging nature of acute NF, clinicians must maintain a high index of suspicion if the patient has suggestive signs and symptoms. In 1990, puppeteer Jim Henson (best known for creating the Muppets) died from NF. At that time, little was known about the progression of group A streptococcal infection.
The disease can quickly cause death, so starting immediate treatment is even more crucial than confirming the diagnosis. Once the disease is suspected, antibiotics must be given immediately and the patient must be prepared for surgery at once. NF spreads rapidly, capable of progressing from a small lesion to death in days to weeks. Thus, delayed diagnosis increases the risk of death. Lack of knowledge about the disease and inability to recognize it promptly are the main reasons many victims die. This article can improve your knowledge base.
Overview
NF was discovered in 1871 by Joseph Jones, a Confederate Army surgeon. At that time, it was called hemolytic streptococcal gangrene, nonclostridial gas gangrene, nonclostridial crepitant cellulitis, necrotizing or gangrenous erysipelas, necrotizing cellulitis, bacterial synergistic gangrene, or synergistic necrotizing cellulitis.
NF involves the fascia, muscle compartments, or both. It can affect not only the muscle fascia but the superficial fascia. NF and cellulitis differ in the amount of tissue involved and extent of tissue involvement.
The most common areas of infection are the abdominal wall, perineum, and extremities. When NF affects the perineum and scrotum, it’s called Fournier gangrene, after the French dermatologist and virologist Alfred Jean Fournier.
The most common causes are trauma, surgery, and insect bites. The disease can affect persons of any age. Such comorbidities as diabetes, chronic renal failure, immunosuppressive therapy, hypertension, obesity, and malnutrition increase susceptibility.
Pathophysiology
NF falls into four classifications based on wound microbiology. Type 1, the most common, involves polymicrobial bacteria. Type 2 results from trauma and is associated with comorbidities. Type 3, rare in this country, stems from gram-negative marine bacteria. Type 4 is a fungal infection occurring mostly in immunocompromised persons. (See Comparing types of necrotizing fasciitis by clicking the PDF icon above.)
Disease progression
The four types of NF progress in a similar way. Bacteria secrete pyrogenic exotoxin A, which stimulates cytokines. These cytokines damage the endothelial lining; fluid then leaks into the extravascular space.
M proteins in streptococci and β-hemolytic streptococci exacerbate the immune reaction by inhibiting phagocytosis of polymorphonuclear leukocytes and normal neutrophil chemotaxis. As the immune reaction increases, blood vessels dilate, allowing toxins to leak through vessel walls, which in turn decreases blood flow. As the cascade continues, hypoxic conditions cause facultative aerobic organisms to grow and become anaerobic. These bacteria exacerbate destruction of surrounding cells and lead to release of carbon dioxide, water, hydrogen, nitrogen, hydrogen sulfide, and methane. As the infection continues to progress, toxins spread throughout the bloodstream and the patient becomes septic.
Assessment
Obtain the patient’s medical history and description of the wound. Determine when the changes first appeared and whether the affected area seemed to get worse recently.
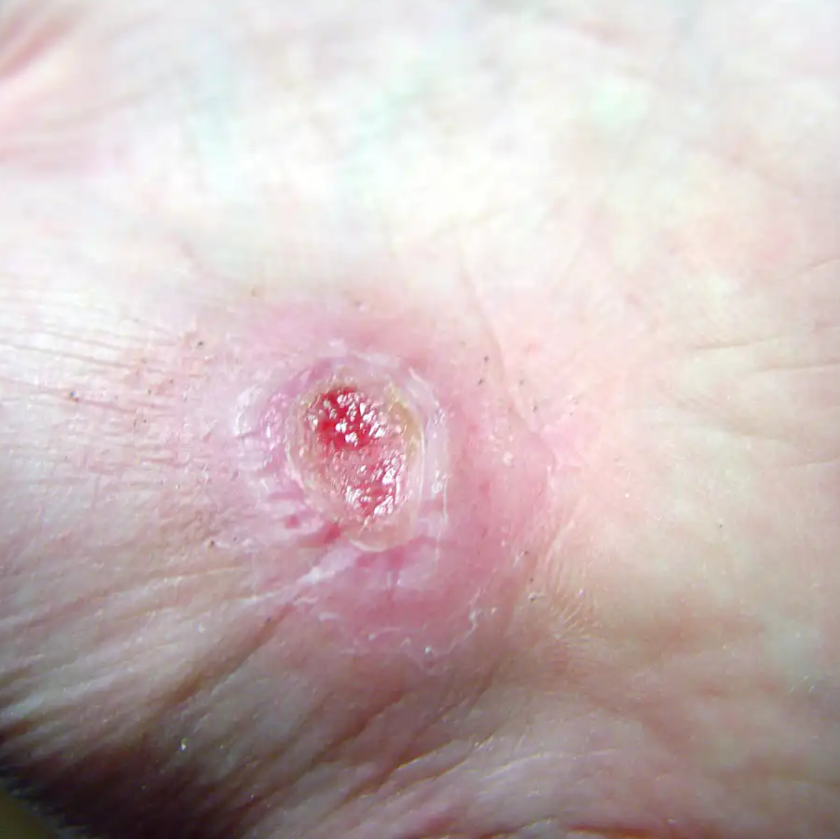
In all NF types, patients commonly present with a small, painful area (possibly with entry marks) but no other signs or symptoms. The wound may appear as a bulla, cellulitis, or dermatitis, representing an infection developing in underlying tissues. The skin may have a wooden-hard feel as the infection progresses to the subcutaneous space and causes necrosis. The wound becomes discolored and necrotic; drainage is rare until surgical debridement begins. The patient quickly develops fever, chills, nausea, and vomiting. As NF progresses, bullae become dark purple with darkened edges; the patient grows disoriented and lethargic, and organ failure and respiratory failure
ensue. Without treatment, the patient dies.
Diagnosis
Diagnostic tests usually include magnetic resonance imaging, complete blood count with differential, comprehensive metabolic panel, and cultures. (See Diagnostic findings in necrotizing fasciitis by clicking the PDF icon above.)
Treatment
Immediate surgical debridement and broad-spectrum antibiotics are needed to stop the immune response to infection. Clindamycin, gentamicin, penicillin, or metronidazole may be given alone or in combination until culture results are available. Supportive care includes total parenteral nutrition for nutritional support, I.V. fluids, and oxygen. Limb amputation should be done only as a last resort.
Surgical debridement involves penetrating deep into the fascia and removing all necrotic tissue. After the first debridement, release of “dishwater fluid” may occur.
Administering hyperbaric oxygen therapy (HBOT) after the first debridement increases tissue oxygenation, thus reducing tissue destruction by anaerobic bacteria. During HBOT (usually given as a 90-minute treatment), the patient breathes 100% oxygen in an environment of increasing atmospheric pressure.
HBOT should be given in conjunction with surgical debridement (usually after each debridement) and should continue until necrotic tissue ceases and cell destruction stops. HBOT also promotes collagen synthesis and neoangiogenesis (new blood vessel growth), which boosts blood supply and oxygen to tissues.
Adverse effects of HBOT include ear pain, oxygen toxicity, and seizures. Ear pain can be minimized by swallowing or yawning. If the patient continues to have ear pain, ear tubes may be inserted by an otolaryngologist. During HBOT, air breaks (intervals of breathing room air) are important in controlling oxygen toxicity (the main cause of seizures).
Throughout the HBOT treatment period, wound dressings must be simple. Well-moistened gauze dressings and an abdominal pad provide good support. Once necrotic destruction occurs, dressings depend on wound size and the need to fill cavities. The patient may require a diverting colostomy, depending on wound
location and the amount of uncontrolled diarrhea. Blood glucose levels must be monitored before and after HBOT, as this treatment affects blood glucose.
Supportive care and follow-up treatment
During initial treatment, patients need supportive care and monitoring. Once they’re out of danger, begin teaching them how to prevent NF recurrences. Advise them to control blood glucose levels, keeping the glycated hemoglobin (HbA1c) level to 7% or less. Caution patients to keep needles capped until use and not to reuse needles. Instruct them to clean the skin thoroughly before blood glucose testing or insulin injection, and to use alcohol pads to clean the area afterward.
Before discharge, help arrange the patient’s aftercare, including home health care for wound management and teaching, social services to promote adjustment to lifestyle changes and financial concerns, and physical therapy to help rebuild strength and promote the return to optimal physical health. One helpful patient resource is the National Necrotizing Fasciitis Foundation. The Centers for Disease Control and Prevention section on necrotizing fasciitis includes “Common sense and great wound care are the best ways to prevent a bacterial skin infection.”
The life-threatening nature of NF, scarring caused by the disease, and in some cases the need for limb amputation can alter the patient’s attitude and viewpoint, so be sure to take a holistic approach when dealing with the patient and family. Today, NF has a much better survival rate than 2 decades ago when Jim Henson died. In my practice, I’ve seen four NF cases. Thanks to early identification, good wound care, and HBOT, these patients suffered only minimal damage.
Selected references
Boyer A, Vargas F, Coste F, et al. Influence of surgical treatment timing on mortality from necrotizing soft tissue infections requiring intensive care management. Intensive Care Med. 2009;35(5):847-853. doi:10.1007/s00134-008-1373-4.
Cain S. Necrotizing fasciitis: recognition and care. Practice Nurs. 2010;21(6):297-302.
Centers for Disease Control and Prevention. Notes from the field: fatal fungal soft-tissue infections after a tornado—Joplin, Missouri, 2011. MMWR. 2011;60(29):992.
Chamber AC, Leaper DJ. Role of oxygen in wound healing: a review of evidence. J Wound Care. 2011; 20(4):160-164.
Christophoros K, Achilleas K, Vasilia D, et al. Postraumatic zygomycotic necrotizing abdominal wall fasciitis with intraabdominal invasion in a non immunosuppressed patient. Internet J Surg. 2007;11(1). doi:10.5580/17a8.
Ecker K-W, Baars A, Topfer J, Frank J. Necrotizing fasciitis of the perineum and the abdominal wall-surgical approach. Europ J Trauma Emerg Surg. 2008;
34(3):219-228. doi:10.1007/s00068-008-8072-2.
Hunter J, Quarterman C, Waseem M, Wills A. Diagnosis and management of necrotizing fasciitis. Br J Hosp Med. 2011;72(7):391-395.
Magel DC. The nurse’s role in managing necrotizing fasciitis. AORN J. 2008;88(6):977-982.
Phanzu MD, Bafende AE, Imposo BB, Meyers WM, Portaels F. Under treated necrotizing fasciitis masquerading as ulcerated edematous Mycobacterium ulcerans infection (Buruli ulcer). Am J Trop Med Hyg. 2012;82(3):478-481.
Ruth-Sahd LA, Gonzales M. Multiple dimensions of caring for a patient with acute necrotizing fasciitis. Dimens Crit Care Nurs. 2006;25(1):15-21.
Stevens DL, Bisno AL, Chambers HF, et al; Infectious Diseases Society of America. Practice guidelines for the diagnosis and management of skin and soft-tissue infections. Clin Infect Dis. 2005;41(10):1373-1406.
Su YC, Chen HW, Hong YC, Chen CT, et al. Laboratory risk indicator for necrotizing fasciitis score and the outcomes. ANZ J Surg. 2008;78(11):968-972.
Taviloglu K, Yanar H. Necrotizing fasciitis: strategies for diagnosis and management. World J Emerg Surg. 2007;2:19.
Lydia Meyers is a medical reviewer for National Government Services in Castleton, Indiana, and a clinical liaison at CTI Nutrition in Indianapolis. She has 11 years of wound care experience in nursing homes, wound clinics, and home health.







One method for fast diagnosis is to perform a bedside surgical cut-down going from skin, sub-cutaneous fat, and through the fascia. With Necrotizing Fasciitis, the fascia is quite weak, compared to normal fascia, and the underlying fluid is the “dishwater” fluid as mentioned in the article. If that is found, the patient needs emergency debridement.
To me, “the prognosis is directly related to the speed of making the diagnosis”.
Thank you for this article.
Remember to maintain 3.5+ Albumin! Lass interstitial fluid load, better circulation. Of course must have adequate vascular network! Merry Christmas
Hello,
My name is Angela Smith and my daughter was diagnosed with Necrotizing Fascitis about 3 years ago. She was working and hit her hand and barely broke the skin and within 24 hours she was fighting for her life she had 2 skin grafts and 12 surgeries on her hand. We we’re transported
by and ambulance to Doctors Hospital in Augusta Ga. My sweet baby my only child was fighting
for her life and was in ICU for 17 days. I am so happy to say she survived this awful bacteria but
unfortunately it left a very bd scar and her only being 23years old at the time was even harder.
The reason that I am writing you is because Iwas wondering if there are any support groups in out area for Survivors of Necrotizing Fascitis in our area Savannah ,GA