By Marcia Spear, DNP, ACNP-BC, CWS, CPSN
Chronic wound infections are a significant healthcare burden, contributing to increased morbidity and mortality, prolonged hospitalization, limb loss, and higher medical costs. What’s more, they pose a potential sepsis risk for patients. For wound care providers, the goal is to eliminate the infection before these consequences arise.
Most chronic wounds are colonized by polymicrobial aerobic-anaerobic microflora. However, practitioners continue to debate whether wound cultures are relevant. Typically, chronic wounds aren’t cultured unless the patient has signs and symptoms of infection, which vary depending on whether the wound is acute or chronic. (See Differentiating acute and chronic wounds.)
With chronic wounds, many clinicians find it more practical to treat local signs and symptoms, such as increased pain and drainage, erythema, friable granulation tissue, and edema. If these are present, a culture is indicated. For a patient with a suspected wound infection, cultures are important in diagnosing the infection, identifying the specific organism, and determining the number of organisms present. This information guides appropriate antibiotic treatment and is crucial in preventing antibiotic-resistant infections.
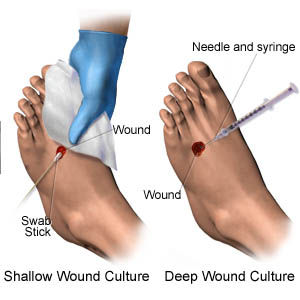
Techniques for obtaining a wound culture
When a wound culture is deemed necessary, what’s the best technique for obtaining it? The current literature on laboratory methods for diagnosing wound infections doesn’t recommend a universal sampling technique or protocol. Three techniques can be used:
• deep-tissue or punch biopsy
• needle aspiration
• swab culture.
Deep-tissue biopsy
A deep-tissue or punch biopsy for a quantitative culture (which determines the colony counts per gram of tissue) is the gold standard for identifying wound bioburden and diagnosing clinical infection. A deep-tissue biopsy after initial debridement and cleaning of superficial debris with normal saline solution is the most useful way to detect invasive organisms. But quantitative biopsies are hard to perform, invasive, painful, expensive, and not available in all settings. Also, they must be done by qualified and trained providers, who aren’t always available.
Needle aspiration
Needle aspiration of wound fluid is a good alternative when there’s little loss of skin, as in puncture wounds or postsurgical wounds with suspected abscess. Data from needle aspirations are reported in terms of colony-forming units per volume of fluid. Although less invasive than tissue biopsy, needle aspiration can be painful and results may underestimate bacterial isolates. Also, exudate must be present in the wound so that aspirate can be collected. Before needle puncture, the area must be cleaned thoroughly with normal saline solution.
Swab culture
In clinical settings, a swab culture is the most common technique used because it’s practical, noninvasive, and cost effective. If done properly, it usually identifies the bacterial species of the infection and helps guide antibiotic therapy. The swab-culture technique for quantifying bacterial burden in burn patients, called Levine’s technique, requires the clinician to twirl the end of the cotton-tipped applicator on a 1-cm2 area of the wound bed with enough pressure to cause minimal bleeding.
The most commonly used alternative to Levine technique is the z-track or 10-point swab culture. This semi-quantitative culture is quick and most useful in a clinical setting. It’s also inexpensive and reproducible. However, it may yield false-positive results, especially if wound-bed cleaning and preparation are inadequate or when only a culture of surface bacteria is obtained. A 2001 prospective study of 38 patients with chronic wounds from various causes evaluated the correlation between quantitative wound biopsies and swab cultures; 27 (74%) of the biopsies indicated infection. Simultaneous swab cultures of these showed infection in 22 cases. The researchers concluded that a quantitative swab culture is a valuable adjunct in managing chronic wounds.
Basic principles for obtaining a wound culture
Although guidelines exist for obtaining a wound culture, no single guideline is used universally. Nonetheless, no matter what technique you use, certain basic principles apply:
• Always obtain the culture from properly cleaned and prepared tissue to avoid obtaining only a culture of surface contamination.
• Collect the culture before topical or systemic antibiotics are initiated.
• Obtain a swab culture from a viable wound bed, as recommended by the Wound Ostomy and Continence Nursing Society guideline. Don’t culture avascular tissue.
Follow these basic steps:
1. Irrigate the tissue with normal saline solution.
2. Moisten a swab with normal saline solution.
3. Swab a 1-cm2 area of viable tissue for 5 minutes with enough force to produce exudate.
Wanted: A clinical practice guideline
The technique used to obtain a wound culture usually depends on the provider and clinical setting. If a clinical practice guideline existed, its use could yield more accurate and complete diagnostic information for true wound infections. The need for a universal evidence-based guideline is apparent.
Selected references
American Society of Plastic Surgeons. Evidence-based clinical practice guideline: chronic wounds of the lower extremity. May 2007. www.docstoc.com/docs/120588469/Evidence-based-Clinical-Practice-Guideline-Chronic-Wounds-of-the-Lower-Extremity. Accessed
December 4, 2013.
Bonham PA. Swab cultures for diagnosing wound infections: a literature review and clinical guideline. J Wound, Ostomy Continence Nurs. 2009;36(4):389-95.
Gardner SE, Frantz RA, Saltzman CL, et al. Diagnostic validity of three swab techniques for identifying chronic wound infection. Wound Repair Regen. 2006;
14(5):548-57.
Kingsley A, Winfield-Davies S. Audit of wound swab sampling: why protocols could improve practice. Prof Nurse. 2003;18(6):338-43.
Levine NS, Lindberg RB, Mason AD, Pruitt BA Jr. The quantitative swab culture and smear: a quick, simple method for determining the number of viable aerobic bacteria in open wounds. J Trauma. 1976;16(2):89-94.
Wound, Ostomy, and Continence Nurses Society (WOCN). Guideline for prevention and management of pressure ulcers. Mount Laurel, New Jersey: Wound, Ostomy, and Continence Nurses Society (WOCN); 2010 Jun 1. www.guideline.gov/content.aspx?id=23868. Accessed December 4, 2013.
Serena T, Robson MC, Cooper DM, Ignatius J. Lack
of reliability of clinical/visual assessment of chronic wound infection: the incidence of biopsy-proven infection in venous leg ulcers. Wounds. 2006;18(7):197-202.
Spear M. Best technique for obtaining wound cultures. Plast Surg Nurs. 2012;32(1):34-6.
Marcia Spear is a nurse practitioner and certified wound specialist in the Department of Plastic Surgery at Vanderbilt University Medical Center in Nashville, Tennessee. She has written numerous articles on wounds and wound care and has lectured to a wide variety of audiences both nationally and internationally.
DISCLAIMER: All clinical recommendations are intended to assist with determining the appropriate wound therapy for the patient. Responsibility for final decisions and actions related to care of specific patients shall remain the obligation of the institution, its staff, and the patients’ attending physicians. Nothing in this information shall be deemed to constitute the providing of medical care or the diagnosis of any medical condition. Individuals should contact their healthcare providers for medical-related information.







I have a primary M.D. and going to be evaluated by wound care doc. I have a small wound (appx. 1/2″ or so long and 1/8/ to 1/4″ wide. It is over my shin where I had a fracture at age 15 (54 now) it was compound so I have scar where my skin was torn. I rec’d septra (allergic to amoxicilin) x 10 days without infection initially. Now after two months due to poor capillary circ from scarring, it is very slow to heal. My primary did a culture yesterday and prelimary reveals “rare PMN’s” awaiting 3 day period. My concern is although I am going to go to a “wound center” soon, I’m from a relatively small town. Secondly, this wound is very close to the tibia due to old compound fx and I also had “chronic” versus acute osteomyelitis (stemming from that fx). This was treated 2 years ago with antibotics and hyperbaric o2. CT scan revealing NO Evidence of Osteo after 1 mo of HBO. I’m generally very careful with my leg, but have had 3-4 skin tears in the past with the last (before this time) tear being prior to finding out I had chronic osteo. Are there any specific questions I should ask wound doctor? Please advise as Im concerned. Thank you.
Deborah,
It is very important that the new wound doctor is familiar with the history of your wound and previous treatments to help with new treatment plans. It could be possible that the osteo is still present but not showing on a traditional x-ray. MRI tests can be used to double check traditional x-rays. http://www.idsociety.org/uploadedFiles/IDSA/Guidelines-Patient_Care/PDF_Library/2012%20Diabetic%20Foot%20Infections%20Guideline.pdf
In addition, underlying circulatory status should be checked if not already completed. Here is link to article that discusses various underlying causes of leg ulcers, not to scare you with these, but it is always important to make sure everything has been ruled out when you have a re-occurring wound. https://www.health.wa.gov.au/WoundsWest/docs/WPR_Nov09_Atypical_Leg_Ulcers.pdf
Hope some of these ideas help you out.
Wishing you good healing!