By Donna Sardina, RN, MHA, WCC, CWCMS, DWC, OMS
Pressure ulcers have been a health concern for a long time—since at least 5,000 years ago, when evidence of a pressure ulcer was found on an ancient Egyptian mummy. But not until 1975 did the staging classification system we’re familiar with begin. This system was designed to make things easier by creating a universal way to describe and communicate the various levels of tissue destruction.
In my travels and work as a wound care educator, the questions I’m asked most frequently relate to pressure ulcer staging. How can this be, given that the staging system was supposed to make it easier for us? Most wound care clinicians who live and breathe wound care 24/7 (the experts) can probably stage a pressure ulcer in their sleep. But the staging struggles of nonexpert clinicians make staging the wound experts’ problem. In many facilities across the country, staging is so challenging that some wound care experts have forbidden anyone else in their facility to document a pressure ulcer’s stage in the medical record. As desirable as this may sound to some of us, I don’t think this approach is practical. One person can’t be everywhere at once.
To stage a pressure ulcer accurately, you need to understand the anatomy and physiology of tissue destruction and be able to interpret what you see. I don’t have all the answers to the staging problem, but I have identified a few issues clinicians find most confusing—differentiating stage II and stage III pressure ulcers, suspected deep tissue injury, and restaging and downstaging. Here are a few tips that may help.
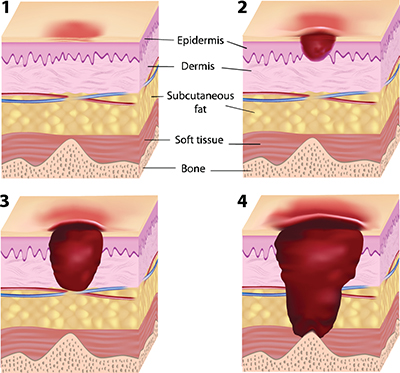
- Stage II pressure ulcers are pink and partial thickness, without necrotic tissue (yellow or black). Tissue destruction is seen through the epidermis and into, but not through, the dermis. (See Stages of pressure ulcers.) In contrast, stage III pressure ulcers involve tissue destruction through the dermis and into the subcutaneous tissue. Of course, there’s no dotted black line showing where epidermis and dermis end, so we have to rely on our knowledge of anatomy: The epidermis is thinnest on the eyelids (0.05 mm) and thickest on the palms and soles (1.5 mm). The dermis is thinnest on the eyelids (0.3 mm) and thickest on the back (3.0 mm). By comparison, a single sheet of copy paper is 0.1 mm thick, while a U.S. penny is 1.5 mm thick.
- A deep tissue injury is a localized area of intact, discolored skin (purple or maroon) or a blood-filled blister. Intact is the key word. Once the skin opens, the wound must be reclassified as unstageable, stage III, or stage IV. Deep tissue injury implies tissue damage at the subcutaneous level or deeper, so it can’t possibly be a stage II wound.
- Reverse or downstaging doesn’t accurately characterize what’s occurring in the ulcer. Stage III and IV pressure ulcers heal by filling in with granulation (scar) tissue—not new dermis and subcutaneous tissue. Therefore, the staging system definitions can be used only one way—as the wound progresses—and not in reverse, as the wound heals. A stage IV pressure ulcer can’t become a stage III, stage II, or subsequently stage I ulcer. When a stage IV ulcer is healing or healed, it should be classified as a healing or healed stage IV pressure ulcer—not a stage I or stage 0 pressure ulcer.
- Progression (worsening) of tissue destruction follows an upward scale of the staging system—from least to worst: stage I, stage II, stage III, and stage IV (the deepest level of tissue destruction). Unstageable and suspected deep tissue injuries are categories, not stages. Based on their definitions, they would be equal to or greater than a stage III ulcer. In other words, they can’t be recategorized as stage I or II ulcers.
- The staging system isn’t perfect and still has many gray areas, but for now this is the internationally accepted tool we need to use. When staging gets confusing or falls into a gray area, I find it’s best not to overthink things. Instead, go back and reread the basic definitions. For answers to other staging questions, check out the article “FAQs for pressure ulcer staging”.
Donna Sardina, RN, MHA, WCC, CWCMS, DWC, OMS
Editor-in-Chief
Wound Care Advisor
Cofounder, Wound Care Education Institute
Plainfield, Illinois
Selected references
National Pressure Ulcer Advisory Panel. The Facts about Reverse Staging in 2000: The NPUAP Position Statement. http://iwa.joerns.com/docs/HTML/education/documents/Facts_about_Reverse_Staging_in_2000.pdf
National Pressure Ulcer Advisory Panel, European Pressure Ulcer Advisory Panel, and Pan Pacific Pressure Injury Alliance. Prevention and Treatment of Pressure Ulcers: Clinical Practice Guideline. Haesler E, ed. Osborne Park, Western Australia: Cambridge Media; 2014.
DISCLAIMER: All clinical recommendations are intended to assist with determining the appropriate wound therapy for the patient. Responsibility for final decisions and actions related to care of specific patients shall remain the obligation of the institution, its staff, and the patients’ attending physicians. Nothing in this information shall be deemed to constitute the providing of medical care or the diagnosis of any medical condition. Individuals should contact their healthcare providers for medical-related information.