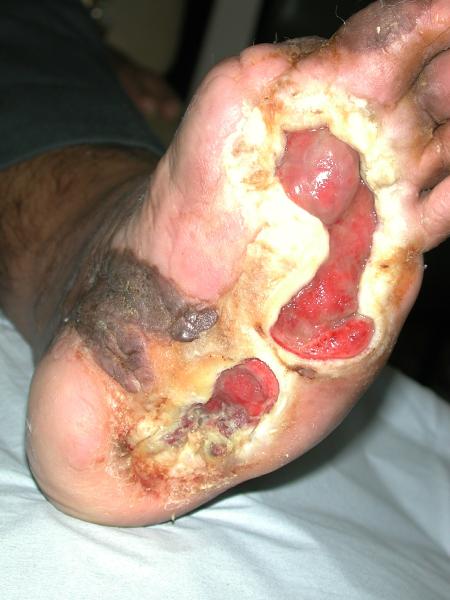
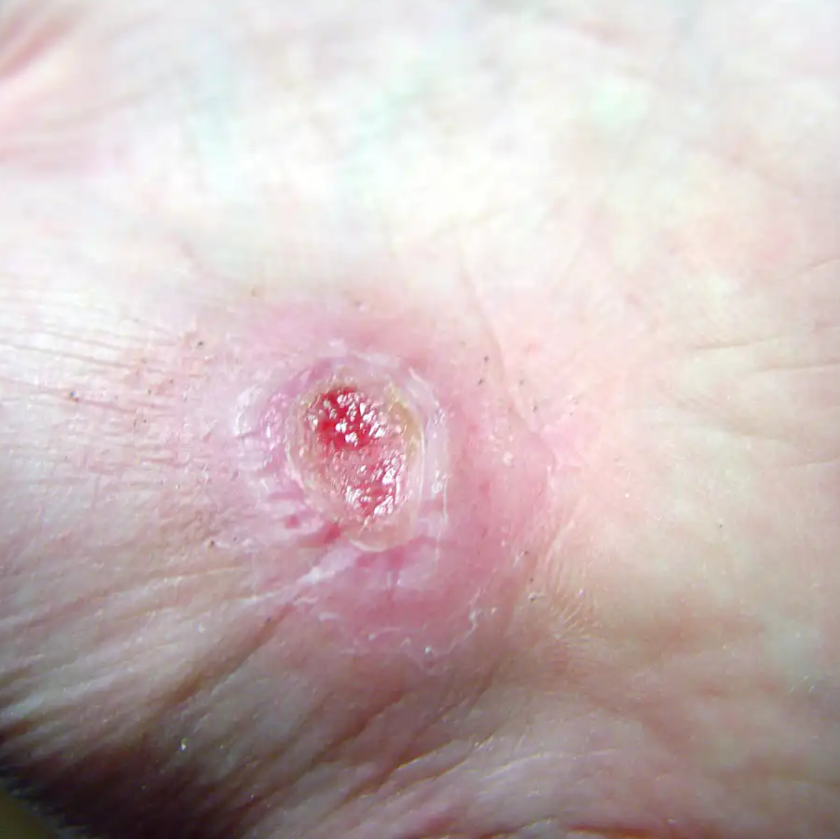
MUNICH — Local injection of mesenchymal stem cells derived from autologous bone marrow shows promise in healing recalcitrant neuropathic diabetic foot ulcers, a novel study from Egypt shows.
Presenting the results at the European Association for the Study of Diabetes (EASD) 2016 Annual Meeting, Ahmed Albehairy, MD, from Mansoura University, Egypt, said: “In patients who received the mesenchymal stem cells, ulcer reduction was found to be significantly higher compared with patients on conventional treatment after both 6 weeks and 12 weeks of follow-up. This is despite the fact that initial ulcer size was larger in the stem-cell–treated group.”
After 6 weeks, median ulcer reductions were 49.9% and 7.67% (P = .001) in stem-cell–treated and control groups, respectively, and after 12 weeks, median ulcer reductions were 68.24% and 5.27% (P = .0001). Complete healing was achieved in one case in the mesenchymal stem cell–treated group.
“The healing mechanism may be due to the pure effect of injected mesenchymal stem cells, which is due to the ability of these cells to simulate angiogenesis in the wound bed, decrease excessive inflammation, and suppress scarring,” explained Dr Albehairy.
In an interview with Medscape Medical News, he said that nearly 10% to 15% of diabetic foot ulcers remain resistant to treatment, with up to a quarter eventually resulting in limb amputation. He noted that several types of stem cells have previously been used to promote healing in diabetic foot ulcers — broadly categorized into allogenic and autologous stem cells — and that mesenchymal stem cells have been used before to successfully treat diabetic critical limb ischemia.
For example, one study from researchers at Tufts University reported earlier this year showed that diabetic foot ulcer–derived fibroblast cell lines can be reprogrammed to a pluripotent state, potentially providing a repository of autologous cells with which to help heal the foot ulcers.
Moderating the session at which Dr Albehairy presented his findings was Andrew Boulton, MD, from the University of Manchester, United Kingdom: “I was slightly concerned that these neuropathic diabetic foot ulcers weren’t easily healed with total contact casts. I wasn’t convinced they had been properly offloaded before entry to the study,” he commented.
Asked whether he thought there was a future in the use of stem cells in healing diabetic foot ulcers, he was cautiously optimistic: “I think we need good properly randomized studies to explore this further.”
Pilot Study Encouraging, but More Work to Be Done
In the current pilot study, Dr Albehairy and his colleagues aimed to study the therapeutic effect of autologous bone-marrow mesenchymal stem cells (adult fibroblastlike cells that can differentiate on exposure to the proper stimulus) on the healing process in patients with neuropathic diabetic foot ulcers.
By study entry, 20 patients from Mansoura Specialized Medical Hospital, Egypt, with resistant neuropathic diabetic foot ulcers had already received 12 weeks of standard-of-care therapy (conventional treatment and proper offloading modalities) but had failed to respond; they were randomized (1:1) to standard of care (n = 10) or standard of care plus locally injected autologous bone-marrow mesenchymal stem cells (n = 10) for a further 12 weeks. Patients in both groups had a mean HbA1c of 8.3% and a mean body mass index (BMI) of approximately 33 kg/m2, and baseline ulcer sizes were 4.66 cm2 and 3.72 cm2 in the investigational and control arms, respectively.
To derive the autologous mesenchymal stem cells, 40 mL of bone marrow was aseptically aspirated from each patient in the mesenchymal stem cell–therapy group. Patients in the control group did not undergo this procedure. After separation, characterization, and subculturing of the stem cells, they were injected into the ulcer site at eight locations on two occasions 7 to 10 days apart. Patients were followed up every 2 weeks up to 12 weeks, which was study end.
“There were no detected complications from bone-marrow aspiration or after the stem-cell injection except for presence of pain during bone-marrow aspiration,” said Dr Albehairy. “These patients had had their ulcers for a long time and were prepared to enter the trial if it offered the potential” for improvement, because their condition seriously affected their quality of life, he explained.
Almost 3.7×105 pure mesenchymal stem cells per cm2 of wound area were injected in all patients in the investigational arm. And “there was a significant correlation between the number of injected cells and percentage of reduction of the ulcer size after 6 weeks and 12 weeks,” he noted.
But he added that there is currently no specific “cutoff” for the number of mesenchymal stem cells required.
“We have a project at Mansoura aimed at detecting the minimum number of stem cells that are required for injection per square centimeter of ulcer to promote healing. This current study is a pilot. We are also looking at mononuclear cells as well as deriving hematopoietic stem cells, with mesenchymal stem cells from adipose tissue as an alternative.”
Drs Albehairy and Boulton have declared no relevant financial relationships .
via medscape.com
European Association for the Study of Diabetes 2016 Annual Meeting; September 13, 2016; Munich, Germany. Abstract 34.