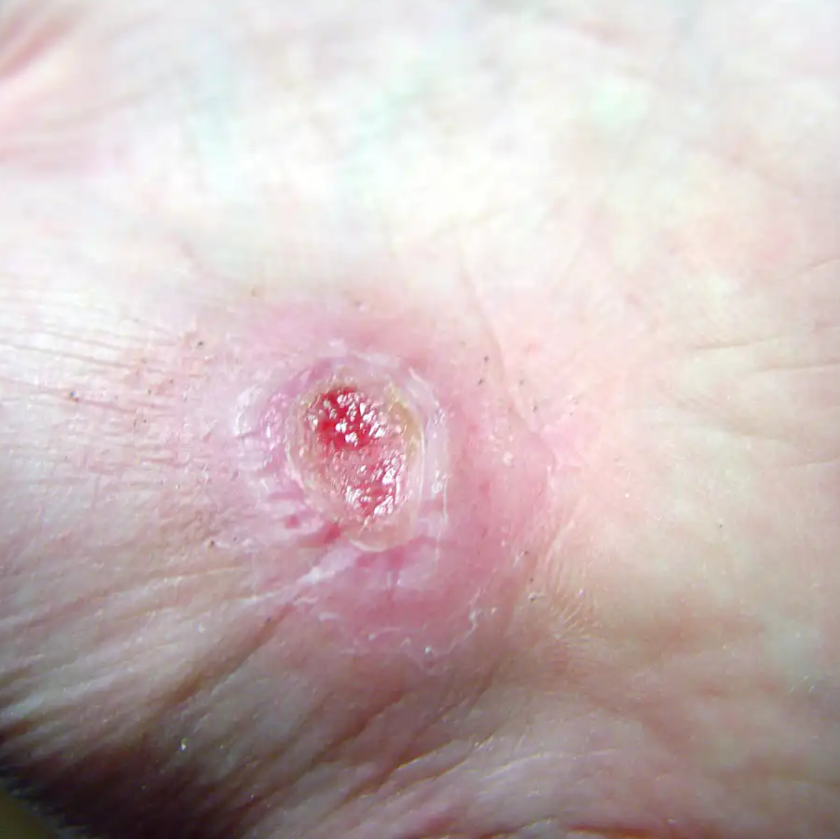
Study finds ultrasound therapy improves venous ulcer healing
In a study of 10 venous ulcers not responding to treatment, the use of noncontact ultrasound significantly reduced the wound area over 4 weeks of treatment.
It has been unclear exactly how ultrasound achieves its positive results. The
authors of “A prospective pilot study of ultrasound therapy effectiveness in refractory venous leg ulcers,” an article published online on February 1 by the International Wound Journal, found that patients treated with ultrasound and compression therapy had reduced inflammatory cytokines and bacterial counts, but the reduction wasn’t statistically significant.
The study found another important benefit for patients-reduced pain.
Serum albumin is not a goodindicator of nutritional status
Traditionally the standard of practice for wound care patients has been to review albumin blood levels as a measure of nutritional status and the effect of nutritional interventions. But as noted in The Role of Nutrition in Pressure Ulcer Prevention and Treatment: National Pressure Ulcer Advisory Panel White Paper, recent studies show that hepatic proteins (albumin, transthyretin, and transferrin) correlate with the severity of an underlying disease, not nutritional status. Moreover, many factors can alter albumin levels even when protein intake is adequate, including infection, acute stress, surgery, cortisone excess, and hydration status.
For these reasons, the National Pressure Ulcer Advisory Panel (NPUAP) and the Academy of Nutrition and Dietetics (previously known as The American Dietetic Association) recommend against using serum proteins as a nutritional assessment tool. Evaluation of lab values is just one part of the nutritional assessment process and should be considered along with other factors such as ensuring that the patient receives what is prescribed; daily food/fluid intake; changes in weight status, diagnosis, and medications; and clinical improvement in the wound.
For more information read “Serum proteins as markers of malnutrition: What are we treating?” and “Albumin as an indicator of nutritional status: Professional refresher.”
A profile of outpatients with wounds
“Wound care outcomes and associated cost among patients treated in US outpatient wound centers: Data from the US Wound Registry” a study using data from the US Wound Registry to determine outcomes and costs for outpatient wound care, found the mean patient age was 61.7 years, slightly more than half (52.3%) were male, most (71.3%) were white, and more than half (52.6%) were Medicare beneficiaries.
Other interesting findings:
- The mean number of serious comorbid conditions was 1.8.
- The most common comorbid conditions were obesity/overweight (71.3%), cardiovascular or peripheral vascular disease (51.3%), and diabetes (46.8%).
- Nearly two-thirds (65.8%) of wounds healed, with an average healing time
of 15 weeks. - In half of the wounds that healed, patients received only moist wound care and no advanced therapeutics.
- The mean cost for wound healing was $3,927.
The authors of the article, published in March’s Wounds, analyzed 5,240 patients with 7,099 wounds in 59 hospital-based outpatient wound centers in 18 states over 5 years.
LOI index comparable to ABI for assessing PAD in patients with type 2 diabetes
The pilot study “Lanarkshire Oximetry Index as a diagnostic tool for peripheral arterial disease in type 2 diabetes,” published in Angiology, compared the gold standard ankle brachial index (ABI) to the Lanarkshire Oximetry Index (LOI) in 161 patients with type 2 diabetes. Researchers assessed the patients for peripheral artery disease (PAD, defined as ABI < 0.9) using both ABI and LOI.
Using a LOI cut-off value of 0.9., the sensitivity and specificity for PAD were 93.3% and 89.1%, respectively. The study concluded that LOI is a “potentially useful alternative diagnostic test for PAD” in patients with type 2 diabetes.
LOI is a noninvasive procedure similar to ABI; both indices indicate whether it’s safe to apply compression to the limb of a patient who has lower leg ulceration or venous hypertension. With LOI, a pulse oximeter is used in place of a hand-held Doppler to determine the index.
Start planning for World Diabetes Day
It’s not too early to begin planning for World Diabetes Day, November 14. Started by the World Health Organization (WHO) and the International Diabetes Federation (IDF), the day is designed to raise global awareness of diabetes.
Access materials, including posters, a campaign book, and the Word Diabetes Day Logo, from IDF’s website, which also has activity ideas.
WHO estimates that more than 346 million people worldwide have diabetes, and the number is expected to double by 2030. World Diabetes Day is celebrated on November 14 to mark the birthday of Frederick Banting who, along with Charles Best, was instrumental in the discovery of insulin in 1922.
Guidelines for PAD in patients with diabetes and foot ulceration published
February’s issue of Diabetes/Metabolism Research and Reviews includes “Specific guidelines for the diagnosis and treatment of peripheral arterial disease in a patient with diabetes and ulceration of the foot 2011,” which is based on two companion International Working Group on the Diabetic foot papers. The guidelines state that if a patient’s PAD is impairing wound healing, revascularization through bypass or endovascular technique must be considered except in a few cases such as severely frail patients. Limb salvage rates after revascularization procedures are about 80-85%, and there is ulcer healing in > 60% at 12 months.
Other points of particular interest to wound care professionals:
- Patients with PAD and a foot infection are at high risk for major limb amputation, so should be treated as a “medical emergency”, preferably within 24 hours.
- Half of patients with diabetes, a foot ulcer, and PAD die within 5 years because of higher cardiovascular morbidity and mortality. Cardiovascular risk management should include “support for cessation of smoking, treatment of hypertension, and prescription of a statin as well as low-dose aspirin or clopidrogel.
AHA statement focuses on PAD in women
“A call to action: Women and peripheral artery disease: A scientific statement from the American Heart Association” summarizes evidence in this area and addresses risk-management issues. The statement notes that women (particularly black females) are more likely than men to experience graft failure of limb loss and calls for more research related to PAD and gender.