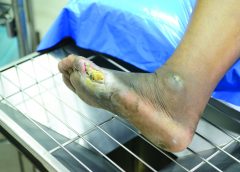
Leg revascularization fails to improve outcomes in nursing home patients
Lower-extremity revascularization often fails to improve outcomes in nursing home patients, according to an article in JAMA Internal Medicine.
“Functional outcomes after lower extremity revascularization in nursing home residents: A national cohort study” found that few patients are alive and ambulatory a year after surgery, and those who are alive have little, if any, gain in function. The study, which included 10,784 patients, was based on data from nursing homes participating in Medicare or Medicaid. (more…)
Read More