By Nancy Morgan, RN, BSN, MBA, WOCN, WCC, CWCMS, DWC
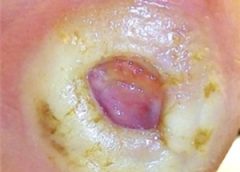
Staging pressure ulcers can get tricky, especially when we’re dealing with a suspected deep-tissue injury (SDTI). The National Pressure Ulcer Advisory Panel defines an SDTI as a “purple or maroon localized area of discolored intact skin or blood-filled blister due to damage of underlying soft tissue from pressure and/or shear. The area may be preceded by tissue that is painful, firm, mushy, boggy, warmer, or cooler as compared to adjacent tissue… Deep tissue injury may be difficult to detect in individuals with dark skin tones. Evolution may include a thin blister over a dark wound bed. The wound may further evolve and become covered by thin eschar. Evolution may be rapid, exposing additional layers of tissue even with optimal treatment.” (more…)
Year: 2017
Exudate amounts
BY: NANCY MORGAN, RN, BSN, MBA, WOCN, WCC, CWCMS, DWC
We’ve talked about types of exudate (drainage). Now let’s consider the amount of exudate in wounds, which is a key part of our assessment.
No exudate present: The wound is too dry.
Scant amount of exudate present: The wound is moist, even though no measurable amount of exudate appears on the dressing.
Small or minimal amount of exudate on the dressing: Exudate covers less than 25% of the bandage. (more…)
Wound exudate types
BY: NANCY MORGAN, RN, BSN, MBA, WOCN, WCC, CWCMS, DWC
What exactly is wound exudate? Also known as drainage, exudate is a liquid produced by the body in response to tissue damage. We want our patients’ wounds to be moist, but not overly moist. The type of drainage can tell us what’s going on in a wound.
Let’s look at the types of exudates commonly seen with wounds. (more…)
Read MoreHow are you differentiating the “big three”?
BY: NANCY MORGAN, RN, BSN, MBA, WOCN, WCC, CWCMS, DWC
Lower extremity ulcers are often referred as the “big three”—arterial ulcers, venous ulcers, and diabetic foot ulcers. Are you able to properly identify them based on their characteristics? Sometimes, it’s a challenge to differentiate them.
Arterial ulcers tend occur the tips of toes, over phalangeal heads, around the lateral malleolus, on the middle portion of the tibia, and on areas subject to trauma. These ulcers are deep, pale, and often necrotic, with minimal granulation tissue. Surrounding skin commonly is pale, cool, thin, and hairless; toenails tend to be thick. Arterial ulcers tend to be dry with minimal drainage, and often are associated with significant pain. The patient usually has diminished or absent pulses. (more…)
Read MoreMeasuring wounds
BY: NANCY MORGAN, RN, BSN, MBA, WOCN, WCC, CWCMS, DWC
An essential part of weekly wound assessment is measuring the wound. It’s vitally important to use a consistent technique every time you measure. The most common type of measurement is linear measurement, also known as the “clock” method. In this technique, you measure the longest length, greatest width, and greatest depth of the wound, using the body as the face of an imaginary clock. Document the longest length using the face of the clock over the wound bed, and then measure the greatest width. On the feet, the heels are always at 12 o’clock and the toes are always 6 o’clock. Document all measurements in centimeters, as L x W x D. Remember—sometimes length is smaller than width. (more…)
ABIs: Do you or don’t you?
BY: NANCY MORGAN, RN, BSN, MBA, WOCN, WCC, CWCMS, DWC
You’ve identified your patient’s lower extremity ulcer as a venous ulcer. It has irregular edges, a ruddy wound base, and a moderate amount of drainage. The patient’s bilateral lower extremities are edematous. As a wound care clinician, you know sustained graduated compression is key to healing stasis ulcers and preventing their recurrence. (more…)
Palliative care patients
BY: NANCY MORGAN, RN, BSN, MBA, WOCN, WCC, CWCMS, DWC
The World Health Organization defines palliative care as care that affirms life and views death and dying as part of a normal process, intends neither to speed nor delay death, provides relief from pain and other distressing symptoms, and offers support to the patient and family. (more…)
Read MoreThink a Patient Has Rights? They Left.
by Dr. Michael Miller
There are few absolutes in my universe. I know that my youngest daughter will gleefully and with full malice (but humorously presented) find something to torment me about every time I see her; referrals from family practice docs arrive well marinated in multiple antibiotics with nary a diagnosis in sight (save for the ubiquitous “infection”); and that regardless of what I recommend, offer, beg, plead, or cajole, that the patient has the complete and total power to make their decisions regarding their care and who provides it. Unless they are deemed by multiple authorities to be incapable of making a decision, until the appropriate paperwork or an emergency situation exists mandating immediate lifesaving action, the ball bounces squarely in their court…or so I thought. (more…)
Read MoreJim Nabors Would Just Cry
by Dr. Michael Miller
For those of you not as familiar with the Hoosier State as you should be, I used to think it was essentially paradise. Jim Nabors of Gomer Pyle fame is our ubiquitous, tuneful icon with his always well-received “Back Home in Indiana” as a mantra to that source of pride. Our former Governor “My Man” Mitch Daniels was a genius who, using a combination of intelligence, common sense and the persuasive powers of a midwest Svengali, created an economic model that our neighbors can only lust after. Our medicolegal climate is among the best in the US and well it should be. However, while there are some extraordinary caregivers and facilities here, a recent US News and World Report curiously showed that almost none of our hospitals made their “Best of” lists in any category. That is not to say there is bad care but to not have a single facility in an entire state even achieve an honorable mention gives one pause to reflect. The State newspapers were notoriously quiet on this concerning fact despite their trumpeting of who does what well, when and where. (more…)
Read MoreHole-ier than Thou, Evidence Based Regardless of the Evidence
by Dr. Michael Miller
There are certain phrases that make the hair on the back of my neck stand up. Someone telling me that they are a good Jew, a good Christian, a good Muslim or the ultimate in self serving lies, “I ONLY practice EVIDENCE BASED MEDICINE”. People who are what they claim they are do not need to announce it. A short conversation, watching them work, others opinions about them all answer the question before it is asked. Like the RN who asked for a recent presentation on the true science behind NPWT (no, you don’t really understand it). She made sure to tell me not only that she practiced only EVIDENCE BASED MEDICINE but then gave me several examples which incidentally had absolutely no scientific evidence (save for articles from lots of dabblers doing lots of crazy things to people and writing about them). I am now awaiting her response as she may have to realize that her version of EVIDENCE BASED is no more real than Kim Kardashian’s celebrity. (more…)
Read MoreIf All You Have is a Hammer, What Happens When You Run Out of Nails?
by Dr. Michael Miller
Over the years of making house calls for wound care, I found that there was a real need for home based mental health and behavioral care, palliative care, podiatry and lots of other things. We cater to those who are home bound based on the classic definition involving the word “Taxing”. One of the more prevalent problems affecting all patients involves the nebulous but ubiquitous, nerve jangling, aptly named, “5th Vital Sign”, namely pain. As a part of my medical group, we have created a program that provides pain management not just to the home bound but all those whose lives and lifestyles are affected adversely by it. The program is a monument to government bureaucracy involving multiple layers of paperwork, mental health evaluations, testing of bodily fluids for both illegal and legal substances and then, the actual evaluation of the patient commences. After all hurdles are vetted and then jumped, then and only then does a prescription for the appropriate nostrum leave the pad. In wound care, we treat based on the etiology, the location, the related factors, the amounts of drainage, the surrounding tissues and so on, ad nauseum. Not surprisingly, in pain management, the scenario is much different. In wound care the mantra of the dabbler is see the hole, fill the hole. In pain management, the goal is to minimize pain to maximize functionality but the overriding questions are how this is accomplished. (more…)
Read MoreCondemning Patients to a Leap of Faith
by Dr. Michael Miller
I have several letters after my name. The two that say “DO” indicate that I have the training of a physician and the requisite education and responsibilities that uphold those letters. They should mean to patients that my ultimate goal is to offer (and provide when the fates allow) the entire spectrum of medical care referable to what I am good at and what they came to seek solace for. Nothing less and if I keep my ego in check, certainly nothing more. Patients run the gamut of their perception of the medical field. But like the old sales nemesis called “Bait and Switch”, what is offered on the sign all too often does not truly match what is seen on the shelves. Arrogant people are that way because they are good at what they do and not afraid to tell others. As a child, we are told to let others brag about us but failing to let people know what we can and can’t do is integral to our patients’ survival and our success. The problem is that the glitz and glamour of being a healer all too often clouds our success. Some time ago, I blogged about the pseudo-utilitarianism of all those so-called “Wound Certification” Exams. At first blush, these seem to be the key to health, wealth, omniscience and outcomes equaled only by those wound care management companies. (more…)
Read More